Mark My Tooth
The Case
A 45-year-old healthy man was scheduled to have two teeth extracted for progressive dental caries. The patient underwent the extractions, awoke from the anesthesia, and then realized that his upper left molars had been extracted instead of his right. The error was recognized and acknowledged immediately following the procedure. The patient still required extraction of the diseased teeth, which occurred a few weeks later. He developed no significant complication from either surgical procedure other than enduring two rounds of anesthesia because of the error.
The Commentary
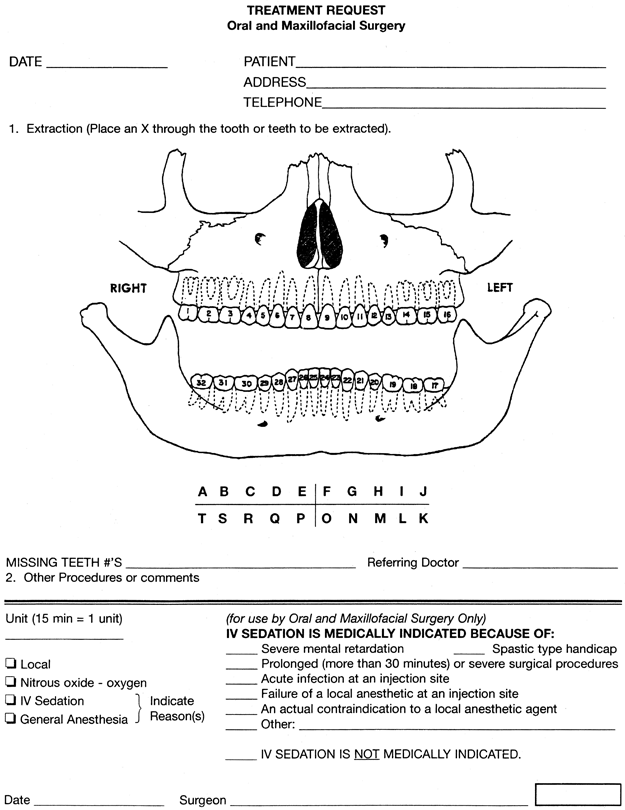
Wrong-site tooth extraction is both a significant medical error and one of the major reasons for litigation against oral and maxillofacial surgeons. This case illustrates a typical scenario where a surgical extraction was performed on the incorrect side. Through a root cause analysis, we might find that the unfortunate event occurred as a result of a cognitive error, the lack of a clear dental diagram (Figure) with the correct teeth marked, an unclear referral slip for the requested services, inadvertent reversal of the radiographs posted on the light box, or disregard of the Universal Protocol. Whatever its cause, once the error is identified, the surgeon should disclose the error and arrange for tooth replacement without any cost to the patient.
Prevalence of Wrong-Site Tooth Extraction
Despite anecdotal reports and known medico-legal implications, few data exist about the prevalence of wrong-site tooth extractions.(1,2) However, most believe that, like other medical errors, these events are under-reported.(3-5) Common etiologies of wrong-site tooth extraction include cognitive failure and miscommunication, multiple contiguous carious teeth (rather than one identifiable diseased tooth), partially erupted teeth mimicking third molars, teeth with gross decay that the restorative dentist wants to save, reversed radiographs, and nebulous tooth numbering systems.
Data from the Oral and Maxillofacial Surgeons National Insurance Company (OMSNIC) Risk Retention Group (Rosemont, Illinois) characterized the nature and extent of wrong-tooth or wrong-site surgery performed by its 4300 members. In the database, the most common reasons for filed claims were paresthesia from third molar extractions and implant placement, infection, and wrong-site tooth extraction. Wrong-site tooth extractions accounted for 14% of all claims and 30% of the claims in which indemnity payments were made. The company identified internal communication problems in the surgeon's office and with the referring dentists as the root causes for many wrong-site surgeries. They also reported no pattern regarding sites and teeth involved in these claims and that the surgeon's age and experience were not important predictors of errors or safety. Unfortunately, no clear trends were identified that would help reduce the number of wrong-site surgeries, and the number of claims has stayed fairly constant despite risk management seminars and online courses sponsored by OMSNIC.
Minimizing the Risk
Most cases of wrong-site tooth extraction can be prevented by the development of an educational program, an informative and unambiguous referral form, a preoperative checklist, and incorporation of the Joint Commission's "Universal Protocol for Preventing Wrong Site, Wrong Procedure, Wrong Person Surgery" into daily clinical practice.
The following comprise the Universal Protocol:
- Preoperative verification process (correct patient, chart, x-ray, referral slip, dental diagram)
- Marking the operative site
- "Time out" immediately prior to beginning the procedure
The American Dental Association (ADA) has supported national efforts to eliminate wrong-site surgery, including wrong-site tooth extraction. However, many of the Joint Commission's safeguards currently in place apply to practitioners in hospitals and ambulatory surgery centers. Very few guidelines or methods for prevention have been established for the primarily office-based practitioners who routinely perform dental procedures. For example, more than 70% of procedures, including dental extractions and other dentoalveolar procedures, occur in this setting.(6)
Improving the safety of tooth extraction and other types of dental surgery begins with a highly reliable preparatory procedure. The process by which dentists and oral and maxillofacial surgeons typically prepare patients for dental extractions in the office setting involves the following steps:
- Review the treatment plan (or if referred, the referral slip) regarding which tooth is to be extracted.
- Review the medical history and record the vital signs.
- Perform the oral evaluation to assess the surgical site.
- Obtain written informed consent (generally, a pre-printed form with a notation of the tooth to be extracted).
- Administer the local anesthesia with or without sedation or general anesthesia.
- Perform the procedure.
- Give postoperative instructions and dispense prescriptions as required.
- Discharge patient when stable and arrange for follow-up.
Recommendations for Safe Practice
In order to improve the quality of care provided in dental offices and avoid dental errors, particularly wrong-site tooth extraction, I would suggest that the following guidelines be followed.
- Develop an educational program for the entire staff on preventing wrong-site tooth extraction. Cognitive failure is the most frequent form of active failure in wrong-site tooth extractions, whereas communication and training represent latent factors contributing to these errors. A carefully designed staff education program may reduce the risk of cognitive failures.(1) Elements of an educational program include case-based materials, information feedback, and clinical guidelines.
- Design a more informative referral slip without ambiguities. Any question or confusion about the correct tooth to be extracted should prompt a call to the referring dentist for clarification. The dentist should also be aware that missing teeth allow for drifting of the remaining teeth into an altered position and can add to potential confusion—particularly if different numbering systems are used to annotate teeth. The ADA recognizes two different tooth numbering systems. The dental practitioner should describe the tooth/teeth to be extracted in longhand (e.g., lower left first molar) on the referral slip and on the consent form, in order to be sure that both the health professionals and the patient understand it.
- Inform the patient/parent/guardian verbally, and with a hand-held patient mirror, which tooth/teeth are to be extracted at the initial consultation appointment.
- Confirm that the patient, chart, and x-ray (properly oriented) are correct and confirm which tooth is to be extracted at the surgical appointment. There is no practical or reliable way to mark teeth prior to the procedure. The Joint Commission and ADA have acknowledged alternatives such as marking the radiograph or a dental diagram visible to the surgeon. A "time-out" should be conducted to confirm the above using the two-person rule. The relationship between the dentist and the hygienist may determine whether the latter can comfortably disagree with the dentist without fear of retribution. The referral form should be checked prior to placing the dental elevator or forceps on the tooth. If there is prosthesis to be inserted after extraction (to replace the extracted tooth), the surgeon should verify that the prosthesis design is compatible with the extraction plan.
Final Thoughts
If a wrong tooth is extracted, regardless of whether the error was identified immediately or delayed, full disclosure and possible remedies must be presented to the patient. Any judgment or settlement that requires a dental licensee or their insurer to pay damages in excess of $3000 because of negligence or error in practice must be reported to the State Dental Board. The Dental Boards also investigate any patient-generated complaints.
Take-Home Points
- Incorporate the preoperative verification process into clinical practice (correct patient, chart, x-ray and its orientation, referral slip, and dental diagram).
- Communicate directly with the referring dentist whenever clarification is required about the procedure requested.
- Use a "time out" immediately prior to beginning the procedure to verify patient, tooth, and procedure with the assistant at the time of extraction (two-person rule).
- Check the tooth position before and after application of the forceps.
Richard A. Smith, DDS Clinical Professor Emeritus University of California, San Francisco
References
1. Chang HH, Lee JJ, Cheng SJ, et al. Effectiveness of an educational program in reducing the incidence of wrong-site tooth extraction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;98:288-294. [go to PubMed]
2. Jerrold L, Romeo M. The case of the wrong tooth. Am J Orthod Dentofacial Orthop. 1991;100:376-384. [go to PubMed]
3. Canale ST. Wrong-site surgery: a preventable complication. Clin Orthop Relat Res. 2005;433:26-29. [go to PubMed]
4. Brennan TA, Gawande A, Thomas E, et al. Accidental deaths, saved lives, and improved quality. N Engl J Med. 2005;353:1405-1409. [go to PubMed]
5. Brennan TA, Leape LL, Laird NM, et al. Incidence of adverse events and negligence in hospitalized patients: results of the Harvard Medical Practice Study I. 1991. Qual Saf Health Care. 2004;13:145-152. [go to PubMed]
6. Perrott DH, Yuen JP, Andresen RV, et al. Office-based ambulatory anesthesia: outcomes of clinical practice of oral and maxillofacial surgeons. J Oral Maxillofac Surg. 2003;61:983. Discussion 995. [go to PubMed]
Figure
Figure. Dental Diagram.
Click on thumbnail for larger view.