Premature or Overdue?
The Case
A 32-year-old woman, gravida 3, para 1, presented for prenatal care at 24 weeks. Her past medical history was unremarkable, and results of her prenatal laboratory tests were normal. On physical examination, she was moderately obese and had a fundal height of 24 cm. Fetal heart tones were about 130 per minute. Routine prenatal care was planned.
The patient missed several ultrasound appointments, but did have several additional prenatal physical examinations that indicated normal growth in fundal height, up to a 41-week size. The physicians recommended that the patient begin post-dates surveillance with twice weekly NST/AFI (Non Stress Test/Amniotic Fluid Index) at 41 weeks, but she missed her first appointment. At 42 weeks, she was admitted for post-dates labor induction using misoprostol and oxytocin. Twelve hours into the induction, examination showed 3 cm cervical dilatation. The patient’s care was handed off to the next day’s labor and delivery team. The team was concerned that the patient had poor dating criteria for post-dates induction and decided to perform an ultrasound examination. The exam showed normal placenta and fluid, and a cephalic singleton with symmetric measurements and estimated fetal weight of 2200 gm, consistent with an estimated gestational age 33 +/- 3 weeks.
The team stopped the induction at this point and observed the patient until her contractions subsided. The next day her cervical examination had regressed to 1 cm dilatation. The team planned to offer amniocentesis or continued twice weekly testing for 3 weeks with follow-up ultrasound for serial growth if undelivered in 3 weeks.
Given the patient’s late entry to care and difficulty keeping ultrasound appointments, the physicians were concerned that she might not return twice weekly for fetal surveillance. An amniocentesis showing fetal lung maturity would permit induction of labor without the risks of loss to follow-up for a possible post-dates or growth-restricted pregnancy. The patient complied with fetal surveillance and delivered a healthy baby boy 3 weeks later.
The Commentary
Approximately 10% of all pregnancies will go postterm.(1) Although the rationale for inducing labor in a postterm pregnancy is a sound one, determining if a pregnancy, such as this one, is truly “postterm” can be difficult.
Definition of Postterm Pregnancy
The definition of prolonged pregnancy endorsed by the World Health Organization (WHO), (1977) and the International Federation of Gynecology and Obstetrics (FIGO), (1986) is 42 completed weeks (294 days or more) from the onset of the last menstrual period (LMP).(2) The etiology of the true postterm pregnancy is unknown. In rare instances, it can be associated with fetal anomalies such as anencephaly or fetal adrenal hypoplasia.
Clinical Significance of Postterm Pregnancies
There is an increased risk of perinatal mortality with postterm pregnancy. In large epidemiological studies, all components of perinatal mortality (that is, antepartum, intrapartum, and neonatal deaths) were increased at 42 weeks and beyond. This finding has been shown to persist despite dramatic improvements in gestational age-specific mortality rates. Increased rates of meconium, shoulder dystocia cesarean delivery, macrosomia (>4500 g), and meconium aspiration were found in postterm deliveries compared with those that delivered at 40 weeks’ gestation.(3)
The accurate determination of the time of conception is pivotal in calculating gestational age and thus in making the diagnosis of postterm pregnancy. In this case, the difficulty encountered was in accurately establishing that this pregnancy was truly postterm. The patient did not start her antenatal visits until 24 weeks gestation and no mention was made as to the certainty of her last menstrual period. At times, a pregnancy may be thought to be postterm when in fact there has been an error in calculating gestational age. For women having 28-day cycles, ovulation tends to occur 14 days following the first day of the last menstrual period. However, if the patient has longer cycles or more specifically a longer proliferative phase, ovulation will occur later. For example, for women having 35-day cycles, ovulation will tend to occur 21 days following the first day of the last menstrual period. Therefore, the calculated estimated date of delivery (EDD) needs to be modified, taking into consideration the length of the cycle. The antenatal forms in Ontario, Canada include a check-box in the area of last menstrual period for cycle length and regularity. If “not regular” is checked, dating should be confirmed by an early ultrasound.
Another component of accurate dating involves ensuring that the gestational age as determined by menstrual history is consistent with the size of the uterus on physical examination and with the time the mother first begins to feel fetal movements. A bimanual examination in the first trimester demonstrating that the size of the uterus is consistent with the gestational age, as determined by menstrual history, is very helpful. Also, the mother usually feels the fetus move at approximately 16-20 weeks. At 20 weeks, the fundal height should be approximately 20 cm above the symphysis and should increase by one centimeter each week. In an obese patient (as in this case), these evaluations will be more difficult to rely on and accurate dating will require ultrasonography. So, despite having a fundal height that seemed consistent with her dates as determined by her menstrual history, an ultrasound should have been done at her first antenatal visit to confirm the accuracy of the gestational age. A prospective study of 764 women found that the incidence of postterm pregnancy was reduced from 10% to 3% when early ultrasound criteria were used to determine gestational age versus relying solely on menstrual history.(4)
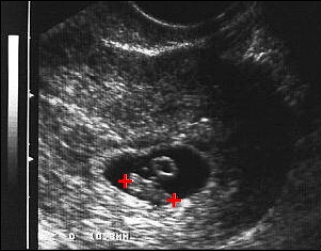
Optimal dating ultrasound is done in the first trimester. From 6 weeks until the end of the first trimester, gestational age correlates closely with the crown–rump length (CRL) (Figure) of the embryo or fetus.(5,6) The accuracy of gestational age determination by ultrasound in the first trimester is +/- 0.5 weeks.(6) After 12 to 13 weeks the CRL becomes less reliable, and in the second and third trimesters, estimation of gestational age depends on a calculated composite of measures of fetal parts. Those most commonly used are the biparietal diameter, the abdominal circumference and the femur length. Fetal measurements become progressively less accurate predictors of gestational age as pregnancy progresses. In the second trimester (between 20 and 26 weeks), the accuracy is +/- 2.1-2.5 weeks. In the third trimester, the accuracy is +/- 3.5-3.8 weeks depending on the measurements available.(7) Consequently, the gestational age that is assigned at the time of the first ultrasound should not be changed later.
In this case, ultrasound assessment could have evaluated fetal well-being in terms of fetal heart rate changes, amniotic fluid volume and uterine artery blood flow velocity. Ultrasound would also have accurately determined the size of the fetus. In retrospect, the findings of a small fetus and no evidence of fetal compromise in this case suggested that the gestational age was possibly less than 37 weeks, and unlikely to be postterm.
Rationale for Management of Postterm Pregnancies
Management of the postterm pregnancy—that is induction of labor versus fetal surveillance—is still controversial. Most clinicians begin surveillance or induction at 41 weeks’ gestation. The rationale for induction of labor comes from several studies. One study randomized 3407 women at 41 weeks or longer to labor induction or fetal surveillance. The investigators were able to demonstrate a significantly lower cesarean rate (21%) in the induction group than the expectant group (24%, p=0.03). The lower cesarean rate in the induction group was due to fewer procedures for fetal distress and dystocia.(8) A meta-analysis of 11 trials looking at induction versus expectant management demonstrated a decreased perinatal mortality (0.3/1000) in the induction group (versus 2.5/1000 in the expectant group). They were also able to demonstrate a decreased cesarean rate in the induction group.(9)
CONCLUSION
In this case, the concept of induction of labor for postterm pregnancy was sound. However, the woman missed several ultrasound appointments scheduled to confirm gestational age. The patient also was not compliant with attempts to begin fetal surveillance. Due to this non-compliance, the real uncertainty about her dates placed the physicians in a difficult bind. Although data support labor induction for significantly post-dates pregnancy, in this case the patient’s true dates were unknown. Prior to inducing labor, fetal heart rate monitoring and an ultrasound assessment of the fetus were warranted. Once the ultrasound showed the fetus was probably premature (and unlikely to be postterm), the management plan was transformed. Instead of considering induction, the physicians now weighed options of either proceeding with an amniocentesis to determine fetal lung maturity prior to further attempts to induce labor, or beginning a program of serial fetal surveillance.
It is important for each new team of caregivers to re-evaluate the clinical situation. In this case, because the referring physician had planned an induction of labor for postterm pregnancy, the on-duty team made the incorrect assumption that accurate dating had occurred. In cases like this one, the first assessment by a new on-duty team should include a reconfirmation of the dating criteria for postterm pregnancy. In this case, a better plan of management would have been developed for the patient if the ultrasound examination had been done before the induction was started. This plan, of course, would not have included an elective induction of labor in a potentially normal preterm pregnancy.
Take-Home Points
Several policies might have prevented the problems seen in this case:
- Perform routine dating ultrasound if the LMP is uncertain or not regular.
- If antenatal care has not begun in the first trimester, a dating ultrasound should be obtained at the first antenatal visit to correlate menstrual dates.
- Dating criteria should be meticulously reassessed prior to labor induction, especially if there has been poor compliance with antenatal care.
- As a method of secondary prevention, each new team should re-examine the specific criteria for labor induction.
Jackie Thomas, MD Mary Hannah, MD Department of Obstetrics and Gynaecology Mount Sinai Hospital and Sunnybrook and Women's College Health Sciences Centre University of Toronto Toronto, Ontario, Canada
References
1. American College of Obstetricians and Gynecologists. Ultrasonography in Pregnancy. ACOG Technical Bulletin No. 187. Washington, DC: ACOG; December, 1993.
2. American College of Obstetricians and Gynecologists. ACOG practice patterns. Management of postterm pregnancy. No. 6. Washington, DC: ACOG; October, 1997.
3. Eden RD, Seifert LS, Winegar A, Spellacy WN. Perinatal characteristics of uncomplicated postdate pregnancies. Obstet Gynecol. 1987;69:296-299.[ go to PubMed ]
4. Reuss ML, Hatch MC, Susser M. Early ultrasound dating of pregnancy: selection and measurement biases. J Clin Epidemiol. 1995;48:667-69.[ go to PubMed ]
5. Robinson HP, Flemming JE. A critical evaluation of sonar "crown-rump length" measurements. Br J Obstet Gynaecol. 1975;82:702-10.[ go to PubMed ]
6. MacGregor SN, Tamura RK, Sabbagha RE, Minogue JP, Gibson ME, Hoffman DI. Underestimation of gestational age by conventional crown-rump length dating curves. Obstet Gynecol. 1987;70:344-8.[ go to PubMed ]
7. Benson CB, Doubilet PM. Fetal measurement-normal and abnormal fetal growth. In: Rumack CM, Wilson SR, Charboneau JW, eds. Diagnostic Ultrasound. 2nd ed. Mosby-Year Book, Inc; 1998:1021.
8. Hannah ME, Hannah WJ, Hellmann J, Hewson S, Milner R, Willan A. Induction of labor as compared with serial antenatal monitoring in post-term pregnancy. A randomized controlled trial. The Canadian Multicenter Post-term Pregnancy Trial Group. N Engl J Med. 1992;326:1587-92.[ go to PubMed ]
9. Crowley P. Postterm pregnancy: Induction of surveillance? In Chalmers I (ed): Oxford Database of Perinatal Trials. Version1.2, disk issue 6, record 4144 Autumn. 1991a.
Figure
Figure. Ultrasound showing crown–rump length (CRL), indicated by (+).