Resuscitation Errors: A Shocking Problem
Edelson DP, Abella BS. Resuscitation Errors: A Shocking Problem. PSNet [internet]. Rockville (MD): Agency for Healthcare Research and Quality, US Department of Health and Human Services. 2007.
Edelson DP, Abella BS. Resuscitation Errors: A Shocking Problem. PSNet [internet]. Rockville (MD): Agency for Healthcare Research and Quality, US Department of Health and Human Services. 2007.
Case Objectives
- Appreciate that delays in defibrillation can have significant negative effects on survival from cardiac arrest.
- List the most common causes of defibrillator failures.
- Appreciate the importance of hands-on, ongoing training on defibrillator devices for users.
- Propose the use of checklists by rescuers at their institution to assess the readiness of the defibrillator and its components.
Case & Commentary: Part 1
A middle-aged man presented to the hospital with chest pain. He was stabilized in the emergency department and admitted to the telemetry ward. He later developed torsades de pointes (an unusual form of ventricular tachycardia that can be fatal if untreated) while on telemetry, associated with loss of his pulse. A code blue was called. The cardiology resident arrived and confirmed torsades on the monitor. Defibrillation pads were placed on the patient, but when the nurse tried to connect the pads to the defibrillation unit, the cables did not connect. In the ensuing confusion, it soon became apparent that the pads and the box were not compatible.
Sudden cardiac arrest (SCA) is a leading cause of death worldwide, claiming more than 300,000 lives each year in the United States alone.(1) SCA presents a difficult clinical problem, as it often occurs with little warning and requires a complex set of resuscitative actions to be instituted within minutes. It is perhaps not surprising, therefore, that survival from cardiac arrest is poor, with out-of-hospital SCA survival to discharge generally reported at less than 10%, and survival from in-hospital SCA estimated at 18% from one large national registry.(2-4)
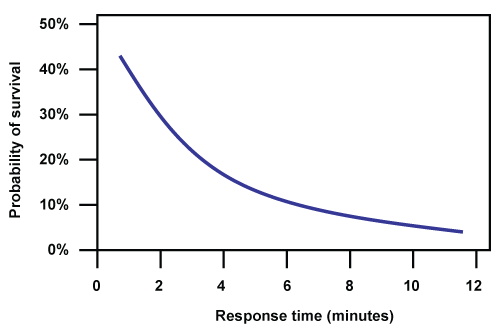
Provided that an electrical shock is applied to the chest quickly, SCA associated with ventricular fibrillation (VF) or ventricular tachycardia (VT) has the best chance of survival. Studies have consistently shown that survival from VF decreases profoundly over the course of minutes in the absence of defibrillation (Figure).(5) Although the provision of cardiopulmonary resuscitation (CPR) ameliorates this effect, this protection wanes quickly. Defibrillation failure rates increase within seconds when CPR is suspended preceding defibrillation.(6)
CPR and electrical defibrillation serve as the essential treatment options for SCA. These therapies are taught to most health care providers, yet performance of these surprisingly complex skills has only recently been objectively measured during actual SCA events and was found to be poor.(7-9) Specifically, CPR parameters are often non-compliant with American Heart Association resuscitation guidelines. Common errors include slow chest compression rates, shallow chest compression depths, hyperventilation, long pauses in CPR before shock delivery, and delivery of electrical defibrillation for non-shockable rhythms. Likely reasons for the variable quality of resuscitation care are infrequent practice of resuscitation skills training by hospital staff and the need for providers to immediately function as a team with others with whom they have not rehearsed.
Unfortunately, defibrillator user errors, such as the one described in this scenario, are not uncommon. In the late 1980s, the Defibrillator Working Group of the U.S. Food and Drug Administration (FDA) reviewed data from the FDA's Medical Device Reporting System (including 1327 reports of defibrillator failures) and from a large number of defibrillator inspections and site visits. They concluded that user errors accounted for most failures and resulted in important defibrillation time delays.(10) Common user errors included holding the defibrillator in a charged state too long (such that the device discharges automatically and requires recharging for actual use), attempting to shock VF in synchronized mode, and inattention to lead selection. These errors have been described in scholarly reviews as well.(11) Additionally, failure to properly maintain and check devices, such that batteries were not properly charged and devices were kept in circulation far in excess of their natural life expectancy of 5–8 years, led to further errors.(10,12) Finally, mismatch of cables with specific defibrillators was described in another published report.(13) Unfortunately, it is often the case that these errors are only noted during an emergency situation, once cardiac arrest has occurred, such that an equipment problem that might have been easily remedied before an event can suddenly present a major hazard to patient survival.
Case & Commentary: Part 2
The patient remained in torsades until the resident administered magnesium, which resulted in rapid conversion to sinus rhythm. The patient was ultimately stabilized and transferred to the cardiac intensive care unit. He suffered no long-term ill effects.
To reduce avoidable errors, as occurred in this case, the Defibrillator Working Group recommended use of a checklist (see Table) by the clinical operators as well as adherence to a maintenance schedule for both the device itself and accompanying batteries. Additionally, they recommended that all defibrillator users receive training in the specific device(s) they are going to use and continued hands-on experience with the device (in cardiac arrests or training) at least every 3 months to maintain those skills. The recommendation for checklists has been echoed by other experts and has been incorporated into the Advanced Cardiac Life Support (ACLS) guidelines.(14-16)
The Defibrillator Working Group found fewer errors in high-use locations such as emergency departments and critical care units, consistent with the notion that increased experience and frequency of device use result in better familiarity and reduced user error.(10) The availability of different defibrillator models in a given hospital has been shown in simulated situations to result in device confusion and increased time to defibrillation.(17) Uniformity of the make and model of defibrillators has been recommended to address these potential problems.(18)
A variety of methods have been proposed to improve resuscitation care, including increasing the frequency of resuscitation skills training and introducing mock SCA events into clinical care routines. Leadership and group training exercises may help improve team function. Routine incorporation of SCA event debriefing can identify common errors and exploit "teachable moments" for further skills improvement. With regard to equipment usage and supply errors such as those described in this case, whenever possible, equipment should be standardized across an institution or health service provider. This is particularly difficult in larger institutions with many distinct cost centers purchasing defibrillators at varying times. In this case, institutional recommendations for devices should be made widely accessible by resuscitation leadership, such as the hospital CPR or "code" committee, so that uniformity can be maintained when an individual clinical unit seeks to replace outdated equipment. All potential rescuers should receive hands-on, device-specific training, with refreshers every 3 months for those in low-use clinical areas.
With regard to equipment problems such as those described by the case in question, a daily (or per shift for high-use areas) equipment checklist should be completed by a member of the resuscitation team or assigned nurse located on a given unit or ward. Specifically, a checklist should be used that ensures that there is no damage to the device, that all components match the device and attach correctly, that the defibrillator battery is charged, and that the device is plugged into wall power for recharging (see Table). Since performing this checklist is a way of familiarizing oneself with the device, as many of the potential rescuers as is reasonable should be taught to perform these inspections and rotate in that responsibility. Biomedical technicians or engineers should perform additional checks every 6 months or as recommended by the manufacturer.
Case & Commentary: Part 3
This incident prompted a major review of code blue procedures, an inventory of the types of defibrillator machines and pads, and an effort to crosscheck machine–pad compatibility. The review resulted in the machines and pads being standardized at this particular hospital, in an effort to eliminate the possibility of this error in the future.
The case detailed here illustrates an all-too-common user error that ultimately reflects a larger systems error. It resulted from having multiple devices in one institution and from failing to use a thorough checklist procedure. Such checklists are a proven tool in such industries as aviation, where a highly complex set of equipment must function correctly with essentially zero tolerance for error. However, it must be emphasized that instituting a checklist is necessary but not sufficient—as in aviation, staff must be educated as to the crucial need to strictly follow checklist procedures and must be motivated to embrace a culture of safety that incorporates such tools. CPR committees at hospitals can serve as crucial champions in this systems approach and should advocate strongly for uniformity of devices and equipment as well as for routine device education and assessment. In this important process, CPR committee members and physician champions for resuscitation care should partner with nurse educators through the hospital system to achieve these objectives. Through such advocacy, resuscitation equipment can become both familiar and safe, and cardiac arrest care can be approached with greater confidence by all members of the hospital team.
Take-Home Points
- Delays in defibrillation can have significant negative effects on survival from cardiac arrest.
- Although most failures to defibrillate are due to user error, they occur in the context of systems problems caused by device confusion and failure to properly maintain defibrillators and their disposable supplies.
- When possible, defibrillators should be standardized within institutions.
- Rescuers should be trained on the device they are going to use and should have frequent hands-on experience with the defibrillator, either in clinical practice or simulations.
- Rescuers should use checklists to assess the readiness of the defibrillator and its components on a daily basis.
Benjamin S. Abella, MD, MPhil Assistant Professor, Department of Emergency Medicine University of Pennsylvania Dana P. Edelson, MD Instructor, Section of General Internal Medicine University of Chicago
Faculty Disclosure: Dr. Abella has received research funding from the NIH, Philips Medical Systems, and Cardiac Science Corporation. He reported a consultant relationship with and speaking honoraria from Philips Medical Systems and speaking honoraria from Zoll Medical Corporation. Dr. Edelson has received research funding and speaking honoraria from Philips Medical Systems and speaking honoraria from Zoll Medical Corporation. The commentary does not include information regarding investigational or off-label use of products or devices. All conflicts of interest have been resolved in accordance with the ACCME Updated Standards for commercial support.
References
1. Thom T, Haase N, Rosamund W, et al, and the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics—2006 update. Circulation. Feb 2006;113:e85-151. [go to PubMed]
2. Eckstein M, Stratton SJ, Chan LS. Cardiac arrest resuscitation evaluation in Los Angeles: CARE-LA. Ann Emerg Med. 2005;45:504-509. [go to PubMed]
3. Lombardi G, Gallagher J, Gennis P. Outcome of out-of-hospital cardiac arrest in New York City: the Pre-Hospital Arrest Survival Evaluation (PHASE) study. JAMA. 1994;271:678-683. [go to PubMed]
4. Peberdy MA, Kaye W, Ornato JP, et al. Cardiopulmonary resuscitation of adults in the hospital: a report of 14,720 cardiac arrests from the National Registry of Cardiopulmonary Resuscitation. Resuscitation. 2003;58:297-308. [go to PubMed]
5. Wik L, Hansen TB, Fylling F, et al. Delaying defibrillation to give basic cardiopulmonary resuscitation to patients with out-of-hospital ventricular fibrillation: a randomized trial. JAMA. 2003;289:1389-1395. [go to PubMed]
6. Edelson DP, Abella BS, Kramer-Johansen J, et al. Effects of compression depth and pre-shock pauses predict defibrillation failure during cardiac arrest. Resuscitation. 2006;71:137-145. [go to PubMed]
7. Wik L, Kramer-Johansen J, Myklebust H, et al. Quality of cardiopulmonary resuscitation during out-of-hospital cardiac arrest. JAMA. 2005;293:299-304. [go to PubMed]
8. Abella BS, Alvarado JP, Myklebust H, et al. Quality of cardiopulmonary resuscitation during in-hospital cardiac arrest. JAMA. 2005;293:305-310. [go to PubMed]
9. Abella BS, Sandbo N, Vassilatos P, et al. Chest compression rates during cardiopulmonary resuscitation are suboptimal: a prospective study during in-hospital cardiac arrest. Circulation. 2005;111:428-434. [go to PubMed]
10. Cummins RO, Chesemore K, White RD, for the Defibrillator Working Group. Defibrillator failures: causes of problems and recommendations for improvement. JAMA. 1990;264:1019-1025. [go to PubMed]
11. Eisenberg MS, Mengert TJ. Cardiac resuscitation. N Engl J Med. 2001;344:1304-1313. [go to PubMed]
12. Emergency Care Research Institute. Hazard: user error and defibrillator discharge failure. Health Devices. 1986;15:340-342.
13. Emergency Care Research Institute. Hazard: mismatch of CCP R2 181-239 cables and HP 43100 defibrillators. Health Devices. 1989;18:233-234. [go to PubMed]
14. Dyson E, Smith GB. Common faults in resuscitation equipment—guidelines for checking equipment and drugs used in adult cardiopulmonary resuscitation. Resuscitation. 2002;55:137-149. [go to PubMed]
15. ECC Committee, Subcommittees and Task Forces of the American Heart Association. 2005 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. Dec 2005;112(suppl 24):IV1-203. [go to PubMed]
16. White RD. Maintenance of defibrillators in a state of readiness. Ann Emerg Med. 1993;22:302-306. [go to PubMed]
17. Sullivan MJ, Guyatt GH. Simulated cardiac arrests for monitoring quality of in-hospital resuscitation. Lancet. 1986;2:618-620. [go to PubMed]
18. Fairbanks RJ, Caplan S. Poor interface design and lack of usability testing facilitate medical error. Jt Comm J Qual Saf. 2004;30:579-584. [go to PubMed]
Table
Table. Defibrillator Checklist
| Inspection Items | OK as Found | Corrective Action/Notes |
|---|---|---|
| 1. Defibrillator a. Clean b. Nothing on top c. No damage 2. Cables/connectors a. Match the device b. Engage securely c. No damage 3. External paddles (including pediatric adapters)* a. Clean, not pitted b. Release from housing easily 4. Internal paddles* a. Match the device b. Sterile 5. Pads* a. 2 sets b. Match the device c. Within expiration date 6. Supplies (verify presence and condition of) a. Electrodes b. Razor c. Spare ECG paper d. Spare battery e. Gel 7. Indicators/ECG Display a. Power "on" b. Self test ok c. Monitor display functional d. "service" message display off e. "Battery charging" light on, "low battery" light off f. Time correct, synchronized with other clocks if possible 8. ECG recorder a. Adequate paper 9. Power supply a. AC/DC cord plugged in b. Spare battery charging c. Rotate batteries per manufacturer recommendations 10. Defibrillation ability a. Charge and discharge per manufacturer recommendations | ||
| Signature_________________________ | Date______ | Time______ |
*If applicable.
Adapted with permission from Elsevier. (Originally published in: White RD. Maintenance of defibrillators in a state of readiness. Ann Emerg Med. 1993;22:302-306.)
Figure
Figure. Survival as a Function of Time to Shock.
Survival from sudden cardiac arrest due to ventricular fibrillation as a function of time from emergency notification to first shock. Adapted with permission from JAMA. Copyright © 2003, American Medical Association. All rights reserved. (Wik L, Hansen TB, Fylling F, et al. Delaying defibrillation to give basic cardiopulmonary resuscitation to patients with out-of-hospital ventricular fibrillation: a randomized trial. JAMA. 2003;289:1389-1395.)