Tough Call: Addressing Errors From Previous Providers
Martinez W, Hickson GB. Tough Call: Addressing Errors From Previous Providers. PSNet [internet]. Rockville (MD): Agency for Healthcare Research and Quality, US Department of Health and Human Services. 2014.
Martinez W, Hickson GB. Tough Call: Addressing Errors From Previous Providers. PSNet [internet]. Rockville (MD): Agency for Healthcare Research and Quality, US Department of Health and Human Services. 2014.
Case Objectives
- Define what it means to be a professional.
- Identify three challenges faced by health care professionals when they uncover potential errors that occurred in the care delivered by their colleagues.
- Review how to balance systems thinking with individual accountability in health care.
- Describe two examples of well-defined processes to identify individual accountability for adverse events and respond to the findings in a measured and fair way.
The Case
A 55-year-old woman with a history of type 2 diabetes on metformin presented to the emergency department (ED) with 3 days of progressive malaise, diffuse abdominal pain, and nausea and vomiting. On presentation, she was afebrile, tachycardic, and hypotensive, with normal oxygen saturation. Her laboratory data was notable for an elevated white blood cell (WBC) count of 23,000/mm3, acute kidney injury with an elevated creatinine of 2.2 mg/dL (up from a baseline of 0.8 mg/dL), and a severe metabolic acidosis secondary to lactic acidosis, with a pH = 7.05 with a lactate of 18 mmol/L (normal 0.5–1.6 mmol/L).
Based on her clinical presentation, she was treated for severe sepsis and given intravenous fluids and antibiotics. In reviewing her medical record, the admitting team noted she had been admitted 3 times in the last 2 months with the identical clinical presentation. Each time she had been diagnosed with sepsis even though no clear source of infection had been found, and each time she had improved and was discharged after 5 days in the hospital. In addition, during two of those hospitalizations, she required mechanical ventilation from pulmonary edema and volume overload from getting aggressive fluids to treat her "sepsis."
The admitting team re-examined all of the information and realized the clinical presentation was not consistent with sepsis; rather, it was far more consistent with acute lactic acidosis secondary to metformin (a well-recognized complication of metformin treatment). The metformin and antibiotics were stopped, and she was treated conservatively and did well. The metformin was added to her allergy list, and, since stopping, she had no further episodes.
The attending physician on the admitting team wondered why the diagnosis had not been made during the previous admissions. Although the degree of illness and lactic acidosis could be consistent with sepsis, no clear source of infection had been discovered; recurrent sepsis without a source is highly unlikely. In addition, the degree of lactic acidosis was out of proportion to the degree of illness, which should have prompted exploration for other causes of severe lactic acidosis (i.e., metformin). She felt like this was a diagnostic error—that the multiple clinicians and teams who had cared for the patient had likely "anchored" on the diagnosis of sepsis and didn't consider other possibilities. She wondered what to do. What was the most effective way to give feedback to the previous teams? Should the providers be blamed for possibly missing the diagnosis? Because the patient likely experienced harm because of the error, should anyone be punished? What could be done to prevent this from happening in the future?
The Commentary
This case illustrates some of the challenges health care professionals face when they discover colleagues may have contributed to an error. In our opinion, the appropriate response of the individual clinician and the health care system should be driven by professional responsibility (i.e., professionalism). This responsibility includes a commitment to cognitive and technical competence in all clinicians, to maintaining behavioral attributes that promote teamwork, and to individual and group regulation (including remediation and potential discipline of members who have failed to meet professional standards).(1)
After discovering a colleague may have contributed to an error, the uncovering professional and organizational leadership face a number of challenges, not the least of which is determining whether and how to disclose the error to the patient or family.(2) Specifically, they must commit to establishing reliable processes and a culture of safety. With this as the goal, the suspected error should be reported to organizational leadership and then analyzed to identify both systems and individual contributions.
The decision to report and address suspected errors contributed to by colleagues can be challenging. However, clinicians in these situations should consider the following questions: If you were the previously treating physician and colleagues suspected an error associated with the care you delivered, would you want to be informed? Would you want to participate in the review? We believe the answers should be "yes" and suggest that without event reporting and professional sharing, it is not possible for the involved professional to engage in self-reflection and self-regulation. It is also impossible for the individual to be a part of addressing the professional duties of disclosure and collaborating to resolve any identified systems problems.
But if you were the involved clinician, how would you want to be made aware? Far too often, physicians tend to talk about each other and not directly to each other, a process known as jousting.(3) Jousting is consistent with the old shame-and-blame culture. Physicians might attempt to avoid potentially awkward or unpleasant conversations with colleagues by using the medical record to call attention to a potential error and to criticize colleagues.(2,3) This approach is inconsistent with professional values (e.g., collegiality, respect, and fairness) because it does not allow the involved colleague to address misunderstandings or provide context, does not facilitate learning, and may be damaging by creating evidence for potentially unnecessary medical malpractice claims.(2,3)
Little empirical data exists on what professionals actually do when they uncover a potential medical error involving a colleague.(2,4,5) However, we know that talking to colleagues who may have contributed to an avoidable adverse outcome is difficult, and physicians, who tend to be focused on the patient's present and future care, may simply choose to remain silent and move on.(4) Informing a colleague that he may have contributed to patient harm may arouse a host of emotions in the involved colleague including anger, fear, shame, and guilt. Ideally, all professionals would receive communication training about how to conduct these challenging conversations. The uncovering clinician will want to choose his words carefully. For example, in a private setting, he might say in a professional and respectful manner, "I want to share with you that Ms. X was readmitted with lactic acidosis. This was her fourth admission, each time with negative cultures. It turned out her lactic acidosis was related to her metformin. I thought you would want know the final diagnosis." Then, the uncovering clinician might pause, listen, and affirm to his colleague that he is an important team member and that is why this information is being shared. This type of quick, nonjudgmental feedback, which we refer to as a cup-of-coffee conversation (6), may motivate appropriate reflection and learning.(7) In the present case, because the diagnosis is rare, it is easier to imagine that the colleague would not feel criticized or ashamed by failing to recognize the diagnosis. However the exchange might be more challenging if a common diagnosis is missed. In addition, the error described in this case both occurred and was uncovered at the same institution. Sometimes errors occurring at one institution are uncovered at another, further complicating the process of communicating with the relevant parties and ensuring appropriate review of, and response to, these events. Despite these added challenges, the principles of professional sharing and reporting of concerns still apply.
Regardless of the nature of the error and its location, appropriate review and feedback is facilitated by a safety culture in which continuous learning is kept front and center. Individuals who work within such a culture expect professional conduct and feel physically and psychologically safe to provide and receive feedback regarding the quality and safety of medical care.(7,8) As professionals, clinicians must be supported in fulfilling their duty to self-regulate by receiving effective feedback and endorsement for practice-based learning.(9) Organizations can reinforce these professional duties by: (i) developing well-defined processes that allow for easy reporting of events, (ii) standardizing performance review and assessment, and (iii) committing to providing feedback early and often to the involved professionals (so continuous feedback becomes expected and not the exception). In addition, organizations should strive to build processes for assessing the extent to which systems and/or individuals contributed to adverse events or near-misses and disseminate this process, thus allowing clinicians to know what to expect.(7) Organizational fidelity to these processes may promote a sense of justice and fairness among all clinicians and make feedback around these events easier to deliver and receive.(7,10)
Applied to the present case, we might imagine organizational processes that incorporate evidence-based tools for identifying possible diagnostic errors, such as a standardized review of all readmissions for the same diagnosis within a defined timeframe.(11) Because these systems for identifying possible diagnostic errors will capture only a fraction of events (11), organizations must rely on individual clinicians to speak up and report suspected missed opportunities and diagnostic errors so cases can be reviewed. In this case, the organization would ideally have a safety culture in which the clinician would feel comfortable (and actually motivated) to report the possible error.
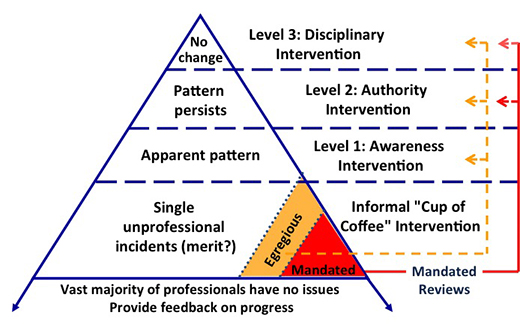
Reason's Unsafe Acts Algorithm (12) and the Professional Accountability Pyramid (6) (Figure) are two tools that can assist medical leaders in identifying individual accountability for adverse events and responding to the findings in a measured way that escalates based on the involved professional's subsequent behavior and performance.
In the present case, Reason's algorithm may define the error as blameless if the involved clinician acted in good faith. However, if the involved professional had a history of unsafe acts, the algorithm recognizes the need for corrective training or counseling.(12) Moreover, even if the clinician is found blameless for the error, this should not imply that his performance was optimal. Clinicians can often learn much by simply reflecting on their performance and the failure to achieve the intended outcome (i.e., earlier diagnosis with avoidance of human and capital costs associated with unnecessary readmissions).
The Professional Accountability Pyramid offers a framework to promote a consistent and proportionate response when the need arises to provide feedback following an avoidable adverse event and/or an unprofessional act.(6) The pyramid outlines a framework for leadership regarding how feedback will be provided and what should be expected from the recipients. For example, in the present case, assume the involved clinician acted as a professional (i.e., was present when needed, performed a history and physical exam, reviewed previous records, was not impaired by drugs or alcohol, and was respectful of other team members who may have suggested alternative diagnoses) and there was no history of similar possible diagnostic errors in the past. In such a circumstance, the event should be considered isolated. The corresponding response would be quick, respectful, nonjudgmental feedback (i.e., cup-of-coffee conversation) similar to what we outlined earlier. No mandates or ultimatums regarding future performance should be made. The cup-of-coffee conversation should recognize that there might remain some uncertainty about the "facts" involved. Acknowledging uncertainty is respectful and decreases distracting and unnecessary arguments. If this occurred in the appropriate culture of patient safety, it would be expected that the involved professional would welcome and appreciate the feedback, reflect about the case or event, and contribute, if possible, to any potential systems fixes.
When a pattern of several misdiagnoses or related safety or quality issues occurs, the Professional Accountability Pyramid directs a measured escalation that would prompt an "awareness" intervention. In this more intensive intervention, a trained peer (or leader) would deliver data "suggesting" that the clinician's care appears to be associated with a disproportionate number of events (or behavior/performance concerns). There is an expectation that the professional self-reflect and self-regulate. For example, the professional may choose to seek out further training, coaching, or continued education, or make changes to their workflow. Follow-up would then occur at a predetermined time to see if the clinician's performance improved. If the professional continues to be associated with a disproportionate number of events or concerns, then a more guided intervention by an authority figure may be necessary. At this level, an authority figure may direct the involved professional to participate in a practice assessment, retraining, coaching, or a comprehensive mental health evaluation. To be effective, these strategies must be employed consistently and without prejudice. Anything less runs the risk of devolving into the old shame-and-blame culture or a belief that the rules apply to some but not others, threatening the trust that is fundamental to a culture of safety.
These processes, focused on individual performance and designed to promote professional accountability, must proceed in parallel with systems-levels processes to reduce the risk of future errors. In the present case, this might include attempts to develop diagnostic checklists or algorithms for common presentations to help ensure clinicians consider all appropriate diagnoses.(13,14)
Balancing systems and individual accountability is critical to the pursuit of a culture of safety. Overemphasizing systems contributions to adverse events risks overlooking important safety threats posed by underprepared, willfully negligent, or impaired individuals. Overemphasizing individual contributions risks overlooking faulty and obsolete systems. A balanced approach helps promote professionalism and a robust safety culture. Professionals within a safety culture are committed to identifying and addressing both systems and human factors that create avoidable risks to patients.
Take-Home Points
- As a professional responsibility, clinicians should commit to cognitive and technical competence, to maintaining the behavioral attributes that promote teamwork (e.g., clear and effective communication, availability, self-awareness, respect, etc.), and to individual and group regulation.
- Organizations should strive to build a culture of safety in which there is a commitment to early reporting of suspected errors. Clinicians should expect to receive continuous feedback on their performance and to engage in analysis of any system-related factors.
- Professional, respectful, nonjudgmental feedback is sufficient to motivate most recipients to reflect and learn from missed opportunities and errors.
- After a suspected diagnostic error, there should be a standardized-review process with well-defined means to: (i) identify both system-level and individual contributions to the error, (ii) communicate findings to the all parties including patients and reporting professionals, and (iii) take corrective action.
- Reason's Unsafe Acts Algorithm and the Professional Accountability Pyramid are two well-defined tools to identify individual accountability for adverse events and respond in a measured and fair way.
William Martinez, MD, MS
Assistant Professor of Medicine
Vanderbilt University Medical Center
Gerald B. Hickson, MD
Senior Vice President for Quality, Safety and Risk Prevention
Assistant Vice Chancellor for Health Affairs
Vanderbilt University Medical Center
Faculty Disclosure: Drs. Martinez and Hickson have declared that neither they, nor any immediate member of their families, have a financial arrangement or other relationship with the manufacturers of any commercial products discussed in this continuing medical education activity. In addition, the commentary does not include information regarding investigational or off-label use of pharmaceutical products or medical devices.
References
1. ABIM Foundation; American Board of Internal Medicine; ACP-ASIM Foundation; American College of Physicians-American Society of Internal Medicine; European Federation of Internal Medicine. Medical professionalism in the new millennium: a physician charter. Ann Intern Med. 2002;136:243-246. [go to PubMed]
2. Gallagher TH, Mello MM, Levinson W, et al. Talking with patients about other clinicians' errors. N Engl J Med. 2013;369:1752-1757. [go to PubMed]
3. Velasco C. Jousting—lighting the malpractice fuse. Minn Med. 2007;90:50-51. [go to PubMed]
4. Grunwald HW, Howard DS, McCabe MS, Storm CD, Rodriguez MA. Misdiagnosis: disclosing a colleague's error. J Oncol Pract. 2008;4:158-160. [go to PubMed]
5. Moskop JC, Geiderman JM, Hobgood CD, Larkin GL. Emergency physicians and disclosure of medical errors. Ann Emerg Med. 2006;48:523-531. [go to PubMed]
6. Hickson GB, Pichert JW, Webb LE, Gabbe SG. A complementary approach to promoting professionalism: identifying, measuring, and addressing unprofessional behaviors. Acad Med. 2007;82:1040-1048. [go to PubMed]
7. Hickson GB, Moore IN, Pichert JW, Benegas M Jr. Balancing systems and individual accountability in a safety culture. In: From Front Office to Front Line: Essential Issues for Health Care Leaders. 2nd ed. Oak Brook, IL: Joint Commission Resources; 2011:1-32. ISBN: 9781599406176.
8. Keroack MA, Youngberg BJ, Cerese JL, Krsek C, Prellwitz LW, Trevelyan EW. Organizational factors associated with high performance in quality and safety in academic medical centers. Acad Med. 2007;82:1178-1186. [go to PubMed]
9. Lesser CS, Lucey CR, Egener B, Braddock CH III, Linas SL, Levinson W. A behavioral and systems view of professionalism. JAMA. 2010;304:2732-2737. [go to PubMed]
10. Reiter CE III, Pichert JW, Hickson GB. Addressing behavior and performance issues that threaten quality and patient safety: what your attorneys want you to know. Prog Pediatr Cardiol. 2012;33:37-45. [Available at]
11. Schiff GD. Finding and fixing diagnosis errors: can triggers help? BMJ Qual Saf. 2012;21:89-92. [go to PubMed]
12. Reason JT. Managing the Risks of Organizational Accidents. Aldershot, Hampshire, England: Ashgate Publishing Company; 1997. ISBN: 9781840141054.
13. Schiff GD, Leape LL. Commentary: how can we make diagnosis safer? Acad Med. 2012;87:135-138. [go to PubMed]
14. Soni K, Dhaliwal G. Misleading complaint. AHRQ WebM&M [serial online]. July 2012. [Available at]
Figure
Figure. Professional Accountability Pyramid. Adapted from (6) with permission of the author.