Silent Pain in the Neck
The Case
A 60-year-old man with no significant past medical history underwent an elective anterior cervical discectomy for persistent right arm weakness due to cervical stenosis. After an uncomplicated procedure, the patient was transferred to a surgical unit with stable vital signs. Later that night, he developed tightness and swelling on the right side of his neck. The nurse notified the covering physician, who asked about stridor or other respiratory symptoms. When told they were absent, he recommended continued close observation. Over the next few hours, the patient's symptoms persisted, and he noted the onset of mild dysphagia. The nurse contacted the in-house intensivist, who evaluated the patient and once again found no evidence of respiratory distress or stridor.
A few hours later, the patient stood up from bed to use the urinal, began coughing, turned cyanotic, and fell to the floor unconscious. Cardiopulmonary resuscitation was started, but the patient's airway was significantly compromised by a now obvious neck hematoma. An emergent tracheostomy was performed at the bedside and the patient was transferred to the intensive care unit.
This postoperative complication led to a prolonged hospitalization. The patient was discharged to a skilled nursing facility, where he required lengthy rehabilitation services.
The Commentary
Postoperative Neck Hematomas
Postoperative hemorrhage is a well-known complication following surgery on the neck and deserves special attention as it can lead to life-threatening acute airway obstruction, as occurred in this case. Although the patient developed a neck hematoma after anterior cervical discectomy, the postoperative course of many commonly performed surgical procedures on the neck, including thyroidectomy, parathyroidectomy, and carotid endarterectomy, can be derailed by this potentially lethal complication. Neck hematoma resulting in airway compromise has also been reported with other commonly performed medical procedures, including central line placement and regional nerve blockade.(1,2)
Anterior cervical discectomy (ACD), carotid endarterectomy (CEA), and thyroidectomy are becoming increasingly routine procedures, and many centers have reduced their lengths of stay in the recovery room and the hospital. Consequently, an increased understanding of the potential complications associated with neck surgery is essential in order to appreciate risk factors for hematoma formation, anticipate the timing for the development of symptoms, and implement strategies for success in maintaining airway patency in patients with airway compromise.
Hematomas may be either superficial (directly below the platysma) or deep (inferior to the deep cervical fascia), with superficial hematomas generally appearing more impressive in terms of neck swelling (Figures). Deeper hematomas are more dangerous as they are less easily detected and require less blood accumulation to cause symptoms. Airway obstruction may result from direct compression of the trachea by a hematoma below the level of the cricoid or from supraglottic edema secondary to venous or lymphatic congestion.(3) At the level of the vocal cords, the cricoid and thyroid cartilages afford protection against external compression by an expanding hematoma. The rate of hematoma expansion may be dependent on the mechanism (e.g., arterial vs. venous bleeding). However, regardless of the mechanism, the interval between hematoma development and airway obstruction may be surprising short.
Epidemiology
The incidence, timing, and risk factors for postoperative neck hematoma are to some extent patient and procedure specific. Nevertheless, some common patterns of postoperative hematoma formation can be identified. The epidemiology of postoperative hematoma formation after ACD, thyroidectomy, and CEA is briefly described below:
Anterior cervical discectomy. The incidence of postoperative wound hematoma after ACD ranges from 1%-11%.(4) Literature on the timing of postoperative hemorrhage after ACD is limited. A recent study of 390 patients who underwent ACD reported an incidence of 1.2% of postoperative hematoma with symptoms of airway obstruction, all of which were diagnosed and evacuated within the first 6 hours after surgery.(5) However, delayed postoperative hemorrhage resulting in airway compromise can occur.(6) Risk factors for postoperative hematoma after ACD include extensive dissection exposing more than three vertebral bodies, a blood loss greater than 300 mL, exposures involving the upper cervical levels, and an operative time exceeding 5 hours.(7) In the case presented, it's unclear which of these factors placed the patient at risk for the life-threatening hematoma that developed.
Thyroid/parathyroid. Several large retrospective studies have reported the incidence of symptomatic hematomas after thyroid and parathyroid surgery to be between 0.1%-1.5%.(8-10) No definite perioperative risk factors have been identified to predict the occurrence of neck hematoma after thyroid and parathyroid surgery. However, numerous possible causes have been proposed, including retching and vomiting during recovery, postoperative hypertension, Valsalva maneuver, intraoperative oozing, preexisting coagulopathy, and bilateral vs. unilateral thyroidectomy.(11) The time interval for development of hematoma after thyroid surgery varies, although most symptomatic hematomas occur within 24 hours of surgery. It is important to emphasize that cases of delayed hemorrhage, occurring 24 hours or more after thyroid surgery, do occur.(12)
Carotid endarterectomy. The incidence of hematoma formation after CEA has been reported to range from 1.4%-5.5%.(13) Risk factors for development of post-CEA hematoma formation include non-reversal of heparin, intraoperative hypotension, general anesthesia, preoperative aspirin use, and placement of a carotid shunt.(14)
Clinical Presentation
Postoperatively, the neck surgery patient should be closely examined for evidence of a developing neck hematoma. Signs and symptoms of an expanding neck hematoma may include respiratory-specific symptoms such as stridor, hypoxia, dyspnea, tachypnea, or tracheal deviation. However, nonspecific symptoms such as change in voice quality, neck tightness, neck pain/pressure, neck swelling, dysphagia, sweating, agitation, and anxiety are often early clinical indicators.
In the case presented, it seems that multiple providers were falsely reassured by the patient's lack of stridor or respiratory compromise and failed to appreciate the early nonspecific signs and symptoms of an expanding hematoma. Additionally, there is no mention that the operative surgeon was called to discuss this patient's complaints. As the individual most familiar with the patient's intraoperative course, the surgeon is best equipped to assess postoperative bleeding risk and decide on a management plan. Such communication may have led to earlier neck re-exploration, thereby preventing airway obstruction and the resulting cardiopulmonary arrest.
Monitoring
Specific protocols for monitoring patients after neck surgery vary across institutions. However, the key components of any effective neck hematoma monitoring protocol include close observation, early detection, and preparation for emergent airway management. Repeated neck circumference measurements are used in some centers, and the physician is notified of any increase in neck circumference. However, due to the compressive nature of soft tissue masses, these measurements may be ineffective in detecting and preventing airway compromise before it is objectively apparent. Ultrasound may have a role in monitoring for neck hematomas, but it has not been systematically studied in this setting. A small incisional dressing, instead of bulky gauze, will allow good visualization of the neck. Diagnosis of a neck hematoma can be particularly challenging after anterior cervical spine surgery due to the presence of a cervical collar, which can obscure otherwise obvious neck swelling. Respiratory arrest due to an unrecognized hematoma under a cervical collar has occurred (15), and a strategy for prevention should include removing the collar periodically to further assess.
Equipment that should be immediately available for bedside use in patients after neck surgery includes a suture removal kit, sterile gloves, and antiseptic solution. Additionally, access to emergency airway equipment and instruments for performing an emergent surgical airway (cricothyrotomy or tracheostomy) should be readily available on the unit. When there are concerns for postoperative bleeding, prolonged observation in a unit with personnel who can provide immediate expert airway management is recommended. Early identification of an enlarging neck hematoma permits successful management in the vast majority of cases.
Management
Hematoma formation resulting from either venous bleeding or an acute hemorrhage of a major artery can cause airway obstruction that must be recognized early and treated with utmost urgency. Airway obstruction can progress from partial to total very quickly, once critical compression from the hematoma impairs venous and lymphatic drainage, leading to laryngopharyngeal edema. In cases of airway obstruction secondary to hematoma, immediate intubation should be performed by an experienced anesthesiologist. While preparing for emergent intubation, decompression of the wound may be a key factor in providing relief from hypoxia and resulting cardiovascular instability.(16) It should be emphasized that mere opening of the platysma may not be sufficient; evacuation of the clot from the tight compartment below the deep fascia is usually required. The surgeon should try to maintain sterile technique where possible by pouring antiseptic solution on the incision, wearing sterile gloves, and using sterile scissors. Bleeding after hematoma evacuation can be managed with gentle pressure once airway patency has been achieved. Intubation may be very difficult, and multiple intubation attempts before opening the wound may aggravate edema, worsening the airway obstruction. In considering how best to perform emergent airway management in this setting, the physician should take into account how the patient was intubated previously, and whether the intubation was difficult. All airway management options (e.g., awake, fiberoptic laryngoscopy, cricothyrotomy) should be considered. Blind intubation techniques may be impossible with neck swelling and potentially traumatize an already compromised airway. It cannot be emphasized enough that this is a high-pressure and risky situation, and the caregivers should ensure that the right team is there for the job—led by the person most experienced in airway management in the building.
In case of inability to intubate, a surgical airway should be performed early. Once the airway is secured, the patient should be sedated and returned to the operating room for safe evacuation of the remaining hematoma, hemostasis, and wound closure.
A conservative approach may be considered in selected patients with minimal hematoma and no progression. Neck hematomas without airway compromise can be managed in a less urgent manner with re-exploration in the operating room. This approach requires careful monitoring of the airway while the patient is being transported to the operating room. The surgeon should be prepared to open the wound immediately if progressive symptoms develop.
Take-Home Points
- Postoperative hemorrhage is a well-known complication following neck surgery that can rapidly lead to life-threatening, acute airway obstruction.
- Nonspecific symptoms such as change in voice quality, neck tightness, neck pain/pressure, neck swelling, dysphagia, sweating, agitation, and anxiety are often early clinical indicators of an expanding neck hematoma. Respiratory-specific symptoms such as stridor, hypoxia, dyspnea, tachypnea, or tracheal deviation occur later.
- If there is evidence of respiratory compromise, the neck wound should be opened immediately and the hematoma should be evacuated to relieve the mass compressing the airway.
- Intubation may be difficult and should be performed by an experienced anesthesiologist. In case of inability to intubate, a surgical airway should be performed early.
- A conservative approach may be considered in selected patients with minimal hematoma and no progression. However, careful monitoring in a unit capable of providing early airway and surgical intervention is essential.
Edward A. Bittner, MD, PhD Program Director, Critical Care Fellowship Associate Director, Surgical Intensive Care Unit Department of Anesthesia, Critical Care, and Pain Medicine
Massachusetts General Hospital
References
1. Kua JS, Tan IK. Airway obstruction following internal jugular vein cannulation. Anaesthesia. 1997;52:776-780. [go to PubMed]
2. Mishio M, Matsumoto T, Okuda Y, Kitajima T. Delayed severe airway obstruction due to hematoma following stellate ganglion block. Reg Anesth Pain Med. 1998;23:516-519. [go to PubMed]
3. Carr ER, Benjamin E. In vitro study investigating post neck surgery haematoma airway obstruction. J Laryngol Otol. 2009;123:662-665. [go to PubMed]
4. Fountas KN, Kapsalaki EZ, Nikolakakos LG, et al. Anterior cervical discectomy and fusion associated complications. Spine. 2007;32:2310-2317. [go to PubMed]
5. Lied B, Sundseth J, Helseth E. Immediate (0-6 h), early (6-72 h) and late (>72 h) complications after anterior cervical discectomy with fusion for cervical disc degeneration; discharge six hours after operation is feasible. Acta Neurochir (Wien). 2008;150:111-118. [go to PubMed]
6. Yu NH, Jahng TA, Kim CH, Chung CK. Life-threatening late hemorrhage due to superior thyroid artery dissection after anterior cervical discectomy and fusion. Spine. 2010;35:E739-E742. [go to PubMed]
7. Sagi HC, Beutler W, Carroll E, Connolly PJ. Airway complications associated with surgery on the anterior cervical spine. Spine. 2002;27:949-953. [go to PubMed]
8. Burkey SH, van Heerden JA, Thompson GB, Grant CS, Schleck CD, Farley DR. Reexploration for symptomatic hematomas after cervical exploration. Surgery. 2001;130:914-920. [go to PubMed]
9. Rosenbaum MA, Haridas M, McHenry CR. Life-threatening neck hematoma complicating thyroid and parathyroid surgery. Am J Surg. 2008;195:339-343. [go to PubMed]
10. Palestini N, Tullett V, Cestino L, et al. Post-thyroidectomy cervical hematoma [in Italian]. Minerva Chir. 2005;60:37-60. [go to PubMed]
11. Bononi M, Amore Bonapasta S, Vari A, et al. Incidence and circumstances of cervical hematoma complicating thyroidectomy and its relationship to postoperative vomiting. Head Neck. 2010;32:1173-1177. [go to PubMed]
12. Lee HS, Lee BJ, Kim SW, et al. Patterns of post-thyroidectomy hemorrhage. Clin Exp Otorhinolaryngol. 2009;2:72-77. [go to PubMed]
13. Shakespeare WA, Lanier WL, Perkins WJ, Pasternak JJ. Airway management in patients who develop neck hematomas after carotid endarterectomy. Anesth Analg. 2010;110:588-593. [go to PubMed]
14. Self DD, Bryson GL, Sullivan PJ. Risk factors for postcarotid endarterectomy hematoma formation. Can J Anaesth. 1999;46:635-640. [go to PubMed]
15. Tew JM, Mayfield FH. Complications of surgery of the anterior cervical spine. Clin Neurosurg. 1976;23:424-434. [go to PubMed]
16. Roy SP. Acute postoperative neck hematoma. Am J Emerg Med. 1999;17:308-309. [go to PubMed]
Figures
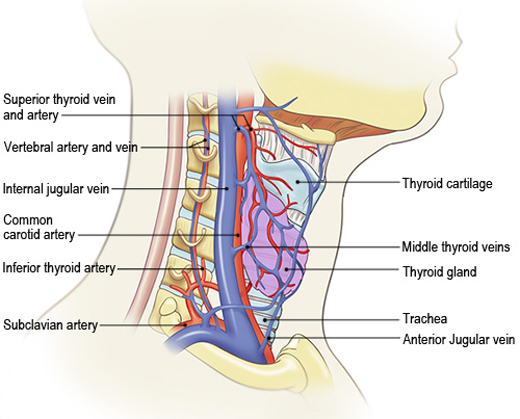
Figure 1a. Structures and vessels of the neck.
(Illustration © 2011 by Chris Gralapp.)
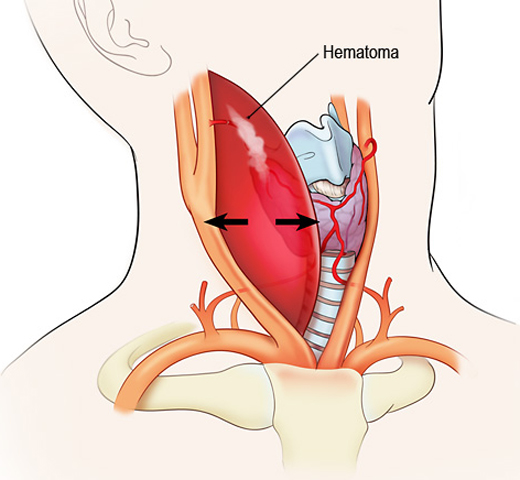
Figure 1b. Expanding neck hematoma with compression of airway.
(Illustration © 2011 by Chris Gralapp.)