Did We Forget Something?
The Case
A 76-year-old-man underwent right aorto-iliac aneurysm repair. He developed postoperative fever, initially attributed to ventilator-associated pneumonia. However, the fever persisted and no definite source was identified. He received multiple courses of broad-spectrum antibiotics over a 2-month hospitalization.
Several months after discharge, he presented to another institution with recurrent fever, neurologic deficits, and renal failure. He was diagnosed as having endocarditis with Candida albicans on the basis of echocardiography and blood culture results. Despite amphotericin and valve surgery, he died a few weeks after this admission.
Autopsy revealed a surgical sponge in the abdomen around the previous aorto-iliac repair. An abdominal computed tomographic (CT) scan during the previous hospitalization had shown a metallic clip in the area of the graft, but no other abnormalities. The patient had not had any other surgeries.
The Commentary
This patient died of a nosocomial candida infection months after an aorto-iliac aneurysm repair. The aneurysm likely was repaired with a prosthetic bypass graft placed during laparotomy. This graft may have become infected and, in addition to the intravascular catheters and antibiotics, could have contributed to the development of an overwhelming fungal infection complicated by endocarditis. Of course, we cannot ignore the possibility that the retained surgical sponge discovered at autopsy contributed to the patient’s infection and eventual demise.
The technical term for "retained sponge" is gossypiboma (from the Latin gossypium, for cotton and the Swahili boma, for place of concealment), but discussions of this issue generally include all types of retained paraphernalia, including surgical instruments, needles, knife blades, electrosurgical adapters, and safety pins. A recent national profile of patient safety indicators in US hospitals between 1995 and 2000 reported a steady decrease in the incidence of foreign bodies left during procedures.(1) However, the true scope of this problem is unknown. Another recent study from a malpractice database in Massachusetts identified 54 patients with retained foreign bodies (roughly two-thirds sponges and one-third instruments).(6) This number corresponds to a statewide event rate of 1 in 9,000 to 1 in 19,000 hospital-based surgical procedures. This estimate implies that a typical large hospital produces at least one case of a retained sponge or instrument each year.
A surgical sponge inadvertently left in the abdominal cavity usually produces one of two responses. It can induce an early foreign body response with an active inflammatory component, whereby the body attempts to extrude the material. This may lead to the development of fistulas. Alternatively, the sponge can induce a fibrinous response that is more indolent, whereby the body creates adhesions and encapsulates the sponge. Patients with this response are at risk for pseudotumors and subsequent symptoms related to obstruction or presence of a space-occupying lesion.(3) Retained sponges have been discovered days, months, and even years after the original operation.(4,5) Even retained surgical instruments have remained undetected for surprising periods of time (though not necessarily without causing symptoms). In late 2002, a Canadian woman set off an airport metal detector and wand, which consistently sounded when placed near her abdomen. She had experienced abdominal pain since surgery 4 months earlier. Several days later, a plain x-ray of the abdomen revealed a 12-inch long, 2-inch wide surgical retractor. Regardless of how retained sponges or surgical instruments are discovered, when recognized they must be removed.(6)
Surgical teams have used sponge, sharp, and instrument counts as protection against this problem for decades. Four separate counts have been recommended: the first when the instruments are set up or sponges unpackaged, a second before surgery begins, a third as closure begins, and the final count performed during subcuticular or skin closure. The purpose of such protocols is that discrepancies at any stage are pursued with repeat counts and, if the discrepancy persists, steps are taken to locate any unaccounted for items. While the practice of sponge counts is a time-honored, simple preventive measure, it is heavily dependent on human performance practices and is thus subject to human error.(7) Anyone who has ever had to recount a pile of coins will recognize the potential problem with this approach. If the "double-check" doesn’t produce the expected number, but a recount does, one simply stops there—ignoring the possibility that the previous discrepancy was correct and that the recount was in error.
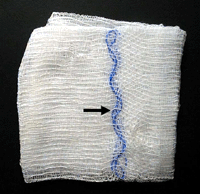
What can be done to prevent this problem? Incorrect counts and incorrect "correct" counts should trigger an adjunctive procedure, such as a portable intraoperative radiograph to detect the presence of the "miscounted" object.(8) However, these additional methods are not universally applied, nor are they failure proof. All laparotomy pads and surgical sponges commercially manufactured in the US have a radio-opaque tail or stripe sewn into the sponge. Sponges placed on the operative field when the operative site is open, and especially those inserted into the thoracic or abdominal cavity, should be radiographically detectable. In the present case, a CT scan was obtained at the time of the initial hospitalization, but the foreign body was not detected.(9,10) The fact that the sponge was not detected may mean one of two things: either the radiologists "missed" the sponge (although the radio-opaque markers used in modern sponges are generally quite obvious [Figure 1 and Figure 2]); or a non-detectable sponge was used at the time of the operation.
Was this patient at high risk for retention of a foreign body after his operation? We have no information about whether sponge counts were performed in this case. A recent retrospective case-control study of medical records associated with claims filed between 1985 and 2001 with a large malpractice insurer in Massachusetts found that patients with retained foreign bodies were more likely to have had emergency surgery, an unexpected change in surgical procedure, or a higher mean body-mass index, and were less likely to have had sponge counts performed at the time of the operation.(2) In this study, failure to perform or complete counts generally occurred in the setting of emergency procedures. Another claims study revealed that in 10% of cases where retained sponges were found, no sponge counts had been performed.(11) It is sobering that so many cases of retained sponges seem to reflect the failure to perform the main strategy for prevention.
Retained sponges and instruments remain a disturbingly common problem, and current preventive practices fail due to human-related factors. Surgeons use non-radiographically detectable sponges, counts are not performed, and when they are performed and errors occur, backup detection systems are not systematically employed. Operating room training and team management skill development may be necessary here (eg, institution of a "time-out for the count" or mandatory intraoperative x-rays for miscounts). Changes to surgical practice and behavior also appear indicated, and new opportunities for technological applications may emerge. Bar-coding or impregnating sponges with detectable sensors would be new ways to improve an old practice. The critical question is not "Was the count correct?" It is "Is there a sponge or instrument in the patient?" Unfortunately, we have yet to identify the best way to answer this question.
Verna C. Gibbs, MD Department of Surgery University of California, San Francisco
References
1. Romano PS, Geppert JJ, Davies S, Miller MR, Elixhauser A, McDonald KM. A national profile of patient safety in U.S. hospitals. Health Aff (Millwood). 2003;22:154-66.[ go to PubMed ]
2. Gawande A, Studdert D, Orav EJ, Brennan TA, Zinner MJ. Risk factors for retained instruments and sponges after surgery. N Engl J Med. 2003;348:229-35.[ go to PubMed ]
3. Lauwers PR, Van Hee RH: Intraperitoneal gossypibomas: the need to count sponges. World J Surg. 2000;24:521-7.[ go to PubMed ]
4. Crossen HS, Crossen DF. Foreign bodies left in the abdomen. St. Louis, Missouri: The C.V. Mosby company; 1940.
5. Gonzalez-Ojeda A, Rodriguez-Alcantar DA, Arenas-Marquez H, et al. Retained foreign bodies following intra-abdominal surgery. Hepatogastroenterology. 1999;46:808-12.[ go to PubMed ]
6. Ibrahim IM. Retained surgical sponge. Surg Endosc. 1995;9:709-10.[ go to PubMed ]
7. Gibbs VC, Auerbach AD. The retained surgical sponge. In: Shojania KG, Duncan BW, McDonald KM, Wachter RM, eds. Making health care safer: a critical analysis of patient safety practices. Rockville, MD: Agency for Healthcare Research and Quality; 2001:255-7. AHRQ publication 01-E058. Evidence report/technology assessment. no. 43. [ go to related site ]
8. Reno D, Lobb J. Recommended practices for sponge, sharp, and instrument counts. AORN Recommended Practices Committee. In: 2000 standards, recommended practices and guidelines: with official AORN statements. 1st ed. Denver, Colorado: Association of operating room nurses; 2000:213-219.
9. Scott WW, Beall DP, Wheeler PS. The retained intrapericardial sponge: value of the lateral chest radiograph. Am J Roentgenol.1998;171:595-597.[ go to PubMed ]
10. Choi BI, Kim SH, Yu ES, Chung HS, Han MC, Kim C. Retained surgical sponge: diagnosis with CT and sonography. Am J Roentgenol. 1988;150:1047-50.[ go to PubMed ]
11. Kaiser CW, Friedman S, Spurling KP, Slowick T, Kaiser HA. The retained surgical sponge. Ann Surg. 1996;224:79-84.[ go to PubMed ]
12. O´Connor AR, Coakley FV, Meng MV, Eberhardt S. Imaging of retained surgical sponges in the abdomen and pelvis. Am J Roentgenol. 2003;180:481-489.[ go to PubMed ]
Figures
Figure 1. Photograph of a 4 x 4 inch surgical sponge. The interwoven radio-opaque marker is visible (arrow).
Reprinted with permission from the American Journal of Roentgenology. (12)
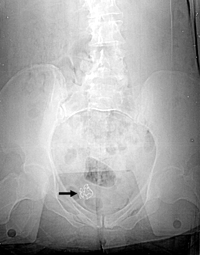
Figure 2. Intra-operative radiograph performed because of an incorrect sponge count in a woman undergoing a urethral suspension (not the present case). The radio-opaque marker (arrow) of a 4 x 4 inch sponge is visible in the pelvis. The sponge was removed before closure.
Reprinted with permission from the American Journal of Roentgenology. (12)