Mistaken Identity
The Case
An 85-year-old Cantonese-speaking woman was admitted to the medical service with altered mental status and a reported fall. After finding tenderness in her left hip, the physicians obtained plain films, which confirmed a nondisplaced femoral neck fracture. The orthopedic surgery team was consulted and, after evaluating the patient, decided that the patient's age, comorbidities, and minimal pain and tenderness on exam made her a candidate for conservative, nonsurgical treatment. These recommendations were documented in her electronic health record, where the team specifically noted: "We're reassured to see the patient is able to weight-bear without pain, even though we wouldn't suggest it in the short-term."
The following day, one of the medical interns read the orthopedic surgeon's note and found these comments about the patient ambulating odd. The patient had strict bed-rest orders and was in significant pain, making it hard to believe that she had been observed walking. After further investigation, the intern realized that the orthopedic team had evaluated the wrong patient—the patient's roommate, who also happened to be a Cantonese-speaking elderly woman. The orthopedic surgery team was consulted again and, after some embarrassment about their mistake, offered surgical repair of the correct patient's fractured hip.
The Commentary
Correctly identifying a patient seems like a straightforward task. However, as this case illustrates, a variety of circumstances may contribute to patient identification errors within complex health care systems. In some cases, incorrect identification may lead primarily to provider embarrassment without any patient harm. Several years ago, I spoke with a physician who was visiting a newly admitted patient seeking treatment for amphetamine addiction. After pulling the curtain around the bed to create an atmosphere of privacy, he began to question the patient about his history of drug use. When the patient denied such abuse, the physician pressed harder, eventually getting the patient to admit to using several illicit substances. As the patient grew increasingly uncomfortable with the conversation, the patient in the neighboring bed finally spoke up and said, "Doc, I think you're supposed to be talking to me." Similar to the case presented, this situation created awkward moments, but ultimately, both patients received the care they required.
On the other hand, many instances of patient identification errors lead to more than embarrassment—such errors can lead to serious harm or even loss of life. These identification errors may occur with phlebotomy, imaging studies or other diagnostic testing, medication administration, delivery of radionuclide agents, blood transfusions, chemotherapy administration, surgeries, and other procedures.(1)
The exact frequency of health care misidentification events is difficult to determine. The United Kingdom Patient Safety Agency reported 236 incidents and near misses in less than 2 years related to missing or incorrect wristbands.(2) The State of New York recorded 27 incidents of invasive procedures on incorrect patients between April 1998 and December 2001.(3) Practitioners in Florida reported 63 wrong-patient surgical procedures between 1990 and 2003.(4) About 0.1% of blood product administrations are associated with an error, with misidentification of the blood recipient accounting for about two thirds of these errors.(5) As reporting systems are often subject to underreporting (3), the real magnitude of this problem is probably greater than these data reflect.
Several patient characteristics may increase the chance of misidentification. Neonates and small children are unable to identify themselves to providers, and family members may not always be present to assist in this process.(6) Communication difficulties caused by dementia increase risk of misidentification in these patients (7); patients with impaired cognition from critical illness, medication effects, or developmental problems may have a similar risk. Our case highlights the impact of language barriers on the potential for patient identification errors. Furthermore, limited English language proficiency, which has been reported in 8% of the population, is also associated with increased risk of serious medical events among both pediatric and adult hospitalized patients.(8,9) All of these characteristics suggest a patient population that could be targeted for prevention strategies.
Environmental factors may also increase the likelihood of patient misidentification. Patients with the same (or similar) names are often found within most health care systems, with up to half of patients in some large systems sharing names with one or more other patients.(10) One study noted that identical surnames were present on 34% of patient days in a neonatal intensive care unit.(11) Adding to the complexity, movement of patients from one inpatient setting to another (e.g., transfer to a different unit or facility) creates opportunities for confusion, as do the growing number of provider handoffs that exist in hospital settings.
Given all of the noted "risk factors" for patient misidentification, a series of prevention strategies has been outlined to mitigate the risk. First, simply checking a patient's wristband to confirm identity is widely viewed as the single most important strategy.(12) Aligned with this step, actively engaging the patient to confirm his or her name as well as a second identifier, such as date of birth, is recommended by the Joint Commission as best practice.(1) The Table provides an example of passive and active patient communication techniques, demonstrating the importance of using an active process. In cases when a patient wristband is removed (e.g., for surgery or IV placement) or has fallen off (e.g., in a neonate), additional steps to ensure correct patient identity are warranted. One of the greatest barriers to recurrent patient identification practices is provider concern that repeated checks will alarm or annoy the patient. Many health care systems are educating all patients and families that their ongoing emphasis on confirming patient identity is part of a commitment to make care as safe and confidential as possible.
Outside of such practices that rely on provider vigilance, specific communication tools, adapted from crew resource management (CRM) practices in aviation, have also been used. For example, the Universal Protocol for Preventing Wrong Site, Wrong Procedure, Wrong Person Surgery requires the use of a "time out" (13) to ensure that all team members are on the same page about the procedure at hand, including assurance of proper patient identification. Similar structured communication techniques and checklists have also been applied outside of procedural areas to improve safety and ensure correct patient identification. Such structured identification and communication practices have been adopted more readily by nurses (particularly in medication administration) but are likely to be equally important in preventing misidentification errors by physicians, as this case vividly demonstrates.
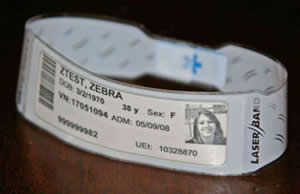
From a technology solution standpoint, the use of bar coding on patient wristbands already plays an integral role in correct patient identification.(14) Adding a patient's picture to the wristband may further improve safety systems by reassuring providers that they are treating the correct patient (Figure). The use of radiofrequency devices has also been suggested as a future strategy for improving patient identification, but such use is not yet widespread.(15) As with other aspects of patient safety, technology will play a key role in improving patient identification systems only if designed and implemented effectively.
Finally, awareness of language barriers should alert providers of the need for an increased focus on proper patient identification and extra attention to communication. If English is a patient's second language, providers may overestimate the amount of information the patient understands. Using interpreter services and taking the time to confirm a patient's understanding of health information will assist in preventing patient misidentification. Ideally, a system—such as an alert, a special designation on a wristband, or an easily identifiable bedside prompt—would be created to assist providers when caring for patients with language barriers.
Take-Home Points
The patient's experience in this case highlights several important lessons about accurate patient identification:
- Patient identification errors occur at least occasionally in virtually every health system, and some lead to significant patient harm.
- Certain patient factors such as young age or impaired sensorium increase the likelihood of misidentification. Use of two patient identifiers is considered best practice.
- Using structured communication tools, such as a preprocedure "time out," is an effective method to ensure appropriate patient identification.
- Technology solutions, including bar coding and radiofrequency devices, may offer additional protection against patient misidentification.
- Language barriers may lead to misidentification and increase the likelihood of adverse events. Identifying patients with such barriers, devoting extra attention to communication, and developing systems for improved interpreter services may all serve as important patient identification strategies.
Leslie W. Hall, MD Senior Associate Dean for Clinical Affairs University of Missouri–Columbia, School of Medicine
References
1. The Joint Commission. Patient identification. Patient Safety Solutions. 2007;1(Solution 2):1-4. Available at: http://www.ccforpatientsafety.org/fpdf/presskit/PS-Solution2.pdf
2. National Patient Safety Agency. Wristbands for hospital patients improves patient safety. Safer Practice Notice 11. 2005:1-6. Available at: http://www.npsa.nhs.uk/nrls/alerts-and-directives/notices/patient-identification/
3. Chassin MR, Becher EC. The wrong patient. Ann Intern Med. 2002;136:826-833. [go to PubMed]
4. Seiden SC, Barach P. Wrong-side/wrong-site, wrong-procedure, and wrong-patient adverse events: are they preventable? Arch Surg. 2006;141:931-939. [go to PubMed]
5. Pagliaro P, Rebulla P. Transfusion recipient identification. Vox Sang. 2006;91:97-101. [go to PubMed]
6. Gray JE, Goldmann DA. Medication errors in the neonatal intensive care unit: special patients, unique issues. Arch Dis Child Fetal Neonatal Ed. 2004;89:F472-F473. [go to PubMed]
7. Miller CA. Communication difficulties in hospitalized older adults with dementia. Am J Nurs. 2008;108:58-66. [go to PubMed]
8. Cohen AL, Rivara F, Marcuse EK, McPhillips H, Davis R. Are language barriers associated with serious medical events in hospitalized pediatric patients? Pediatrics. 2005;116:575-579. [go to PubMed]
9. Bartlett G, Blais R, Tamblyn R, Clermont RJ, MacGibbon. Impact of patient communication problems on the risk of preventable adverse events in acute care settings. CMAJ. 2008;178:1555-1562. [go to PubMed]
10. Lee AC, Leung M, So KT. Managing patients with identical names in the same ward. Int J Health Care Qual Assur Leadersh Health Serv. 2004;18:15-23. [go to PubMed]
11. Gray JE, Suresh G, Ursprung R, et al. Patient misidentification in the neonatal intensive care unit: quantification of risk. Pediatrics. 2006;117:e43-e47. [go to PubMed]
12. Beyea SC. Systems that reduce the potential for patient identification errors. AORN J. 2002;76:504-506. [go to PubMed]
13. The Joint Commission. Universal protocol for preventing wrong site, wrong procedure, wrong person surgery. Available at: http://www.jointcommission.org/PatientSafety/UniversalProtocol/
14. Murphy MF, Kay JD. Barcode identification for transfusion safety. Cur Opin Hematol. 2004;11:334-338. [go to PubMed]
15. Kondro W. American Medical Association boards implantable chip wagon. CMAJ. 2007;177:331-332. [go to PubMed]
Table
Table. Comparison of Passive and Active Communication Techniques for Confirming Patient Identification
| Passive Communication | Active Communication |
|---|---|
| Physician: Good morning, Mrs. Jones. I'm sorry to awaken you. My name is Dr. Brown, and I'm from the Orthopedic Department. Your physician asked that I stop by to visit with you and briefly examine you this morning. Patient: Okay. | Physician: Good morning; I'm sorry to awaken you. Patient: That's okay. Physician: My name is Dr. Brown from the Orthopedic Department. Can I take a moment and ask you to confirm your name? [Looks at name band.] Patient: I'm Sarah Jones. Physician: And can you confirm your date of birth for me? [Still looking at name band.] Patient: March 4, 1936. Physician: Thank you, Mrs. Jones. We always like to make sure we're talking to the right patient before we begin to discuss important medical information. Is this a good time to visit with you about your recent fall and hip injury? Patient: It's fine, doctor. |
Figure
Figure. Example of patient wrist band using patient name, date of birth, bar coding, and patient photo as aids to proper patient identification.