Postdischarge Follow-Up Phone Call
Mourad M, Rennke S. Postdischarge Follow-Up Phone Call. PSNet [internet]. Rockville (MD): Agency for Healthcare Research and Quality, US Department of Health and Human Services. 2012.
Mourad M, Rennke S. Postdischarge Follow-Up Phone Call. PSNet [internet]. Rockville (MD): Agency for Healthcare Research and Quality, US Department of Health and Human Services. 2012.
Case Objectives
- Understand why preventing readmissions through postdischarge phone calls is important.
- Describe evidence supporting postdischarge phone calls.
- List important steps in implementing a postdischarge phone call program.
- List common pitfalls when establishing a postdischarge phone call program.
The Case
A 63-year-old woman with a history of chronic obstructive pulmonary disease (COPD) presented with several days of a productive cough, shortness of breath, and fever. Based on her clinical history, physical exam, and diagnostic studies, she was diagnosed with community-acquired pneumonia and admitted to the hospital. She was treated with ceftriaxone and doxycycline, intravenous fluids, and supportive care. The patient improved rapidly over 48 hours and was discharged home (she lived with her daughter and grandson) with a prescription for doxycycline (an oral antibiotic) to complete a 7-day course and guaifenesin for a persistent cough.
Over the next few days following discharge, the patient's cough worsened, and the shortness of breath returned despite taking antibiotics. She called her primary care physician (PCP) to schedule an urgent appointment, but he was out of the country, and no appointments were available in the clinic. She also vaguely remembered being given a number at the hospital to call if she had any issues at home, but she could not locate the number in the large stack of papers she was given at discharge. As her symptoms worsened, she contemplated returning to the emergency department (ED).
That afternoon, she received a phone call from the hospital where she had been discharged. At this hospital, all patients discharged from the medicine service are called by a nurse within 3 days. The nurse asked a standard list of questions and learned about the worsening symptoms.
The nurse contacted the discharging team regarding the worsening cough and shortness of breath. The team was concerned that her pneumonia was returning and she was failing the doxycycline treatment. They contacted her local pharmacy and were able to prescribe levofloxacin (a broader spectrum antibiotic). The patient's daughter was able to get the prescription the same day and the patient began taking the levofloxacin.
The nurse who had called previously called again 2 days later to check on the patient. With the change in antibiotics, the patient felt much better with improving symptoms. She did not need to return to the hospital and was able to see her primary care doctor 2 weeks later. The discharging team was convinced that the follow-up phone call by the nurse had definitely prevented a return visit to the ED and potentially a readmission to the hospital.
The Commentary
The period following hospitalization remains a particularly vulnerable time for patients. Multiple studies have shown that adverse events occur in approximately 1 in 5 patients.(1,2) Unfortunately, readmission to the hospital after discharge is common—nearly 20% of hospitalized older Medicare patients will be readmitted within 30 days.(3) Some of these readmissions may be planned, whereas others may be part of the natural evolution of disease and treatment. But, many hospitalizations owe to errors in diagnosis, consequences of treatment (most commonly adverse drug events), and worsening symptoms.(2,4) There is a widespread belief that some, perhaps most, readmissions, can be prevented by changing the way care is provided across transitions of care.
Transitional care, or the care patients receive as they move across health care settings and providers, involves bridging care gaps across different health care settings, including ED visits, hospitalizations, and outpatient visits.(5) Hospital-based transitional care interventions aim to smooth the transition from the inpatient to the outpatient setting and (hopefully) prevent unplanned readmissions. Many strategies have been employed to avoid preventable adverse events after discharge and prevent rehospitalizations, including patient engagement in discharge planning, a transitions coach (a provider, often a nurse, who is responsible for coordinating the transition), communication with outpatient providers, timely follow-up appointments, home visits, and postdischarge telephone calls.(6-8)
Preventing readmissions is important—for the patient, the providers, the hospital, and the health care system. The Patient Protection and Affordable Care Act (PPACA), the health care law passed in 2010, includes provisions focused on decreasing preventable readmissions and improving the quality of care during this transitional period. Under this legislation, hospitals will be financially penalized for high readmission rates. The Centers for Medicare & Medicaid Services now publicly report hospitals' risk-adjusted 30-day readmission rates for specific diagnoses on its Web site, Hospital Compare (http://www.hospitalcompare.hhs.gov). Financial penalties aside, readmissions can be quite costly, and they carry the potential for harm to the patient, including missed work, missed time with family, further deconditioning, and exposure to hospital-associated complications. Preventing a readmission thus not only saves the hospital money, but can also improve the health of the patient in the long term. Hospitals and health care organizations therefore have considerable incentives to improve transitions of care, and interventions to improve transitions are becoming widespread.(9)
This case illustrates the potential benefits of one of these interventions: postdischarge phone calls. The patient developed worsening symptoms after discharge and was unable to reach her PCP. For most patients, the next step would be a visit to the ED or urgent care setting. However, a nurse-initiated phone call soon after discharge used a focused script to elicit these symptoms and was able to contact the discharging team. With prompt action by the discharging team and an engaged family, a visit to the ED and likely a readmission were prevented. A phone call by a trained hospital-based provider allows for direct contact with the patient or caregiver in less time and at less cost to the hospital than a home visit. These calls aim to identify and resolve postdischarge issues such as problems understanding discharge instructions, problems obtaining outpatient appointments, problems filling prescriptions, issues relating to medication management, and new or worsening symptoms.(10-12)
In the last two decades, there has been substantial research evaluating the benefit of postdischarge telephone calls, either as part of a multicomponent transitional care program or as a separate intervention. Most of the successful transitional care programs, including the Transitional Care Model (6), the Care Transitions Intervention (7), and Project RED (8), employed calls after discharge as part of a multimodal intervention. Unfortunately, most of the data evaluating postdischarge calls as an independent intervention are of poor methodological quality, with low patient numbers and high risk of bias (13), and their results have been mixed. Many of the interventions focus on certain diagnoses or localized groups of patients, including patients with congestive heart failure (CHF), surgical patients, or patients in the ED. The primary and secondary outcomes have also varied across the studies—they have included patient satisfaction, reduction in medication errors, and effect on readmissions or repeat ED visits. Telephone follow up in patients with CHF was associated with fewer hospital days and readmissions in the 6 months following the index hospitalization.(14) A pharmacist-initiated telephone follow-up program after hospital discharge demonstrated reduced visits to the ED within 30 days of discharge.(10) However, other studies in ED patients using a nurse liaison and large telephone follow-up program at a tertiary care medical center with medical–surgical patients led to improved patient satisfaction but had no effect on readmission rates or adverse events.(15,16)
Despite the heterogeneity of the published studies and mixed results, we still believe there are real benefits to implementing a postdischarge phone call program. Postdischarge phone calls allow hospital and outpatient providers to identify and remedy possible gaps that may be occurring from hospital admission through discharge. Postdischarge phone calls also allow providers to reinforce key elements of the discharge instructions, medication changes, and follow-up plans for patients who are doing well. In this case, the phone call was able to mobilize resources to address concerning symptoms occurring after discharge. At our institution, phone calls have been credited with the prevention of many adverse events. For example, nurses recently discovered that a newly diagnosed diabetic was administering long-acting insulin three times daily (should only be used once daily) and were able to follow up to prevent a hypoglycemic event. Nurses also contacted a young patient who had been hospitalized with a new diagnosis of Crohn disease and discovered she was unable to get the expected follow up in the gastrointestinal clinic due to insurance problems. They were able to help get her an appropriate clinic appointment. An analysis of the 2240 phone calls made in 2011 at our institution found that nurses assisted patients in almost 50% of calls. The main interventions have been (i) providing education regarding medications and discharge instructions (38%), (ii) assisting with follow-up appointments (36%), and (iii) following up on symptoms after discharge (43%). Although postdischarge phone calls were not specifically mentioned in the Transitions of Care Consensus Policy Statement (17), they have been a part of nearly every large successful transitions intervention.(6-8)
Based on our experience and our review of the literature, there are several key steps to ensuring a successful postdischarge phone call program.
- Identify a provider to make the calls. It is important that providers making calls are resourceful, follow through on patient concerns, and are able to recognize worrisome symptoms that require an escalation of care. Little data exist to guide provider selection. Nurses, pharmacists, and case managers have all been employed to make calls.(6-8,16,18,19) Given that most adverse events after discharge involve medications (1), it would seem reasonable to consider pharmacists first. However, hospitals may choose to use nurses or case managers based on available resources and institutional culture.
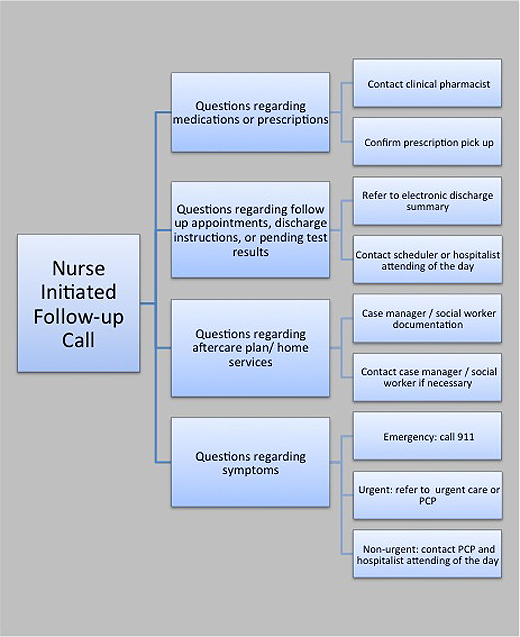
- Create a resource network to troubleshoot issues raised on the call. Possible partners include nurses, physicians, case management, home care, primary care physicians, and pharmacists. A postdischarge phone call provider should have an algorithm (Figure) to help efficiently triage issues after discharge within their resource network.(12)
- If possible, provide a call-back number for patients who you cannot reach and can leave a message. Leaving your name, call-back number, and critical information such as follow-up appointment information can make the call more effective.
- Develop a script that can best elicit patient concerns with a mix of closed and open-ended questions. "How are you taking your Lasix?" may uncover more issues than "Do you have any questions about your discharge medications?"(20)
- Ensure access to the EMR (if possible) for the person making the calls. This can be key in obtaining information about discharge medications, plans for follow-up appointments, and home services. Ensure that call providers can easily identify and reach parties, such as the discharging team, the patient's primary care provider, or home care providers.
- Track call outcomes to help inpatient providers learn from issues addressed in the call. Phone calls should feedback the most common preventable postdischarge issues back to the inpatient physicians and staff.
When starting a call program, it is useful to be aware of potential pitfalls of this intervention. A provider who lacks adequate training or support to intervene on postdischarge issues may actually increase visits to the ED, potentially increasing readmissions. For example, a patient experiencing chest pain after an endoscopy might be sent immediately to the ED by an inexperienced provider, while a more seasoned provider might ask questions to determine whether the pain is more concerning for a cardiac versus gastrointestinal cause. Continuity of care with the PCP may also suffer in a poorly organized system of postdischarge phone calls. Many phone call programs are provided by hospitals, which may exclude PCPs or home care providers from knowledge regarding key events or medication changes after discharge. It is important to include primary providers in any communications or changes stemming from the call.
The first step in determining the resources needed to support the calls is understanding the volume of patients to be called and the time needed per call. Given the dearth of strong evidence linking follow-up phone calls to decreased readmissions, some programs may choose to target only high-risk patients, for example, elderly patients, those with certain diagnoses, or those discharged on multiple new medications. According to published studies, most postdischarge phone calls take 10 to 20 minutes.(16) However, if issues arise after discharge, the time needed to adequately address issues may be much longer. In estimating the time for a follow-up phone call program, it is important to include the time pharmacists, physicians, and case managers spend in troubleshooting, as well as the time needed to aggregate and summarize the issues raised in the calls to feedback to frontline providers.
Postdischarge phone call programs, like the one employed in this case, allow hospital providers a simple and effective way to identify and intervene on issues that may arrive after discharge. This case illustrates how a scripted, well-resourced phone call program can be used to reduce adverse events after discharge and potentially prevent readmissions.
Take-Home Points
- Transitional care interventions, such as postdischarge phone calls, can reduce adverse events and readmissions after discharge, which are costly to both patients and hospitals.
- Little solid evidence exists linking follow-up phone calls (when viewed as an isolated intervention) to reduced readmissions, but postdischarge phone calls have been a part of nearly every successful transitions program.
- An effective follow-up phone call program employs providers who can recognize postdischarge issues and utilizes a network of providers to intervene on behalf of the patient.
- A formal script to elicit questions and concerns, a method to document the communication in the medical record, and a connection with primary care providers can improve the success of the calls.
Michelle Mourad, MD
Assistant Clinical Professor of Medicine
Division of Hospital Medicine
University of California San Francisco Medical Center
Stephanie Rennke, MD
Assistant Clinical Professor of Medicine
Division of Hospital Medicine
University of California San Francisco Medical Center
Faculty Disclosure: Drs. Mourad and Rennke have declared that neither they, nor any immediate member of their families, have a financial arrangement or other relationship with the manufacturers of any commercial products discussed in this continuing medical education activity. In addition, the commentary does not include information regarding investigational or off-label use of pharmaceutical products or medical devices.
References
1. Forster AJ, Murff HJ, Peterson JF, Gandhi TK, Bates DW. The incidence and severity of adverse events affecting patients after discharge from the hospital. Ann Intern Med. 2003;138:161-167. [go to PubMed]
2. Forster AJ, Clark HD, Menard A, et al. Adverse events among medical patients after discharge from hospital. CMAJ. 2004;170:345-349. [go to PubMed]
3. Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009;360:1418-1428. [go to PubMed]
4. Epstein K, Juarez E, Loya K, Gorman MJ, Singer A. Frequency of new or worsening symptoms in the posthospitalization period. J Hosp Med. 2007;2:58-68. [go to PubMed]
5. Naylor MD, Aiken LH, Kurtzman ET, Olds DM, Hirschman KB. The care span: the importance of transitional care in achieving health reform. Health Aff (Millwood). 2011;30:746-754. [go to PubMed]
6. Naylor MD, Brooten D, Campbell R, et al. Comprehensive discharge planning and home follow-up of hospitalized elders: a randomized clinical trial. JAMA. 1999;281:613-620. [go to PubMed]
7. Coleman EA, Parry C, Chalmers S, Min SJ. The care transitions intervention: results of a randomized controlled trial. Arch Intern Med. 2006;166:1822-1828. [go to PubMed]
8. Jack BW, Chetty VK, Anthony D, et al. A reengineered hospital discharge program to decrease rehospitalization: a randomized trial. Ann Intern Med. 2009;150:178-187. [go to PubMed]
9. National Quality Forum (NQF). Measurement Framework: Evaluating Efficiency Across Patient-Focused Episodes of Care. Washington, DC: NQF; 2009.
10. Dudas V, Bookwalter T, Kerr KM, Pantilat SZ. The impact of follow-up telephone calls to patients after hospitalization. Am J Med. 2001;111:26S-30S. [go to PubMed]
11. Koehler BE, Richter KM, Youngblood L, et al. Reduction of 30-day postdischarge hospital readmission or emergency department (ED) visit rates in high-risk elderly medical patients through delivery of a targeted care bundle. J Hosp Med. 2009;4:211-218. [go to PubMed]
12. Rennke S, Kesh S, Neeman N, Sehgal NL. Complementary telephone strategies to improve postdischarge communication. Am J Med. 2012;125:28-30. [go to PubMed]
13. Mistiaen P, Poot E. Telephone follow-up, initiated by a hospital-based health professional, for postdischarge problems in patients discharged from hospital to home. Cochrane Database Syst Rev. 2006;4:CD004510. [go to PubMed]
14. Riegel B, Carlson B, Kopp Z, LePetri B, Glaser D, Unger A. Effect of a standardized nurse case-management telephone intervention on resource use in patients with chronic heart failure. Arch Intern Med. 2002;162:705-712. [go to PubMed]
15. Jones JS, Young MS, LaFleur RA, Brown MD. Effectiveness of an organized follow-up system for elder patients released from the emergency department. Acad Emerg Med. 1997;4:1147-1152. [go to PubMed]
16. Bostrom J, Caldwell J, McGuire K, Everson D. Telephone follow-up after discharge from the hospital: does it make a difference? Appl Nurs Res. 1996;9:47-52. [go to PubMed]
17. Snow V, Beck D, Budnitz T, et al. Transitions of Care Consensus policy statement: American College of Physicians, Society of General Internal Medicine, Society of Hospital Medicine, American Geriatrics Society, American College of Emergency Physicians, and Society for Academic Emergency Medicine. J Hosp Med. 2009;4:364-370. [go to PubMed]
18. Schnipper JL, Kirwin JL, Cotugno MC, et al. Role of pharmacist counseling in preventing adverse drug events after hospitalization. Arch Intern Med. 2006;166:565-571. [go to PubMed]
19. Fitzgerald JF, Smith DM, Martin DK, Freedman JA, Katz BP. A case manager intervention to reduce readmissions. Arch Intern Med. 1994;154:1721-1729. [go to PubMed]
20. Marvel MK, Epstein RM, Flowers K, Beckman HB. Soliciting the patient's agenda: have we improved? JAMA. 1999;281:283-287. [go to PubMed]
Figure
Figure. Post Discharge Follow-Up Phone Call Algorithm