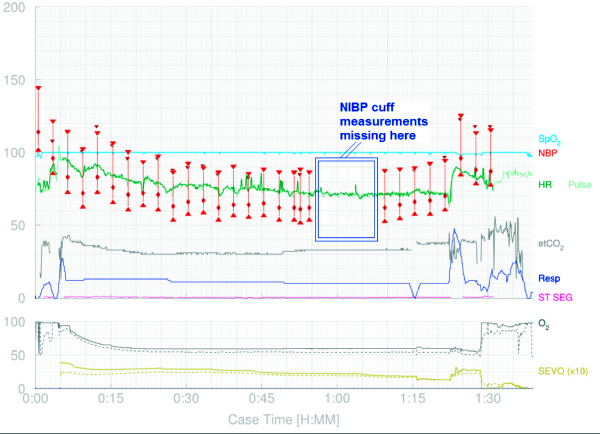
No BP During NIBP
The Case
An otherwise healthy 49-year-old man with atrial fibrillation was scheduled for ablation in the catheterization laboratory under general endotracheal anesthesia. The procedure lasted 7 hours. Per American Society of Anesthesiologists guidelines, monitoring included continuous electrocardiography, oxygen saturation, end tidal carbon dioxide, as well as noninvasive blood pressure (NIBP) measurement every 5 minutes. The patient was extremely stable with values hardly changing over time. Inadvertently between 4 PM and 5 PM, the NIBP stopped "cycling," but this was not recognized. When the attending anesthesiologist took over the case at the end of the certified registered nurse anesthetist's (CRNA) shift, she noticed that the "graphic trends" tab on the monitor had a straight line for heart rate and oxygen saturation (indicating no change over time) and a blank space for the NIBP. A lookup of numerical trend was done and it showed that the last NIBP recording was more than 60 minutes earlier. After discovering the error, the case continued without any problem. The patient was extubated and discharged home the next day as planned. The patient was informed about the mistake and he accepted it as human error.
Reviewing the case revealed that certain safety checks that are routine in the operating room (OR) do not routinely occur in the cardiac catheterization laboratory setting in this hospital. First, OR attending physicians are expected to frequently check the progress of the case. Second, the automated anesthesia record in the OR shows "blank" if there are no new NIBP recordings. Third, the OR doctors' work area has a central monitor feed that the attendings watch when they do paperwork. Fourth, the OR monitors "gray" out NIBP value if the cuff is not cycling. These features are not in place for out-of-OR cases. In addition, the monitor for the catheterization laboratory was a different make and model from those in the OR, and the CRNA was unfamiliar with the menu and knobs. The anesthesia record was manual, and the CRNA kept documenting the same reading for a whole hour. Human factors such as fatigue and lack of vigilance in a very stable case also contributed to the error.
The Commentary
In the presented case, the certified registered nurse anesthetist (CRNA) neglected to cycle the noninvasive blood pressure (NIBP) cuff for more than 1 hour during an atrial fibrillation ablation procedure in the catheterization laboratory. This meant that a significant period of time passed with no new blood pressure values being measured; however, the patient's blood pressure was documented as unchanged in the anesthetic record. Gaps of more than 10 minutes between successive blood pressure measurements are quite common, occurring in 1.5%–7% of all anesthetics.(1) Although the patient in this case did not appear to experience any harm from this lack of vigilance (2), this conclusion cannot be definitive as the patient's blood pressure was not known during this monitoring window. Moreover, the fact that the patient likely had no serious adverse effects was good fortune—had the blood pressure fallen during the procedure and the clinicians remained unaware, serious harm could have resulted. This error is a near miss.
A second error in this case was that the previous ("stale") blood pressure value was documented as a new measurement, reflective of the current state of the patient's physiology, when in fact no new measurement had been obtained. Documenting a value when it wasn't measured is the opposite of the commonly occurring problem where a measurement or clinically relevant observation was not documented. Lack of documentation is more prevalent during manual record-keeping than with electronic data capture.(3)
The American Society of Anesthesiologists standard for patient monitoring during anesthesia is independent of location. It simply states that "During all anesthetics, the patient's oxygenation, ventilation, circulation and temperature shall be continually evaluated" and requires blood pressure measurements at least every 5 minutes.(4) Given the common remoteness of other areas in which anesthesia is given—such as intervention radiology and the cardiac catheterization laboratory—from the general operating rooms, it may be advisable to have extra emergency equipment and an additional anesthesia professional close at hand (5), as support from the core anesthesia locations may not be readily available enough in the event of an emergency. Indeed, there is a higher risk of adverse outcomes in these locations which could be prevented with the use of better monitoring.(6)
As in this case, the anesthesia machines and patient monitors in the non-operating room setting are often of different makes, models, and configurations than those in the core operating room locations.(7) Lack of familiarity with equipment may have contributed to the CRNA's oversight of the lapse in NIBP cuff cycling and consequent update of values on the monitor, as the patient monitor behaved differently than the monitors commonly used in the operating rooms. It is quite possible that a user intimately familiar with this patient's monitor would have identified, and rectified, this problem immediately—as did the attending anesthesiologist. Insufficient familiarity with equipment has long been recognized as a contributing cause for preventable incidents (8), and combined with other human error may result in patient harm.(9) Finally, over-reliance on automated technology may give a false sense of security and safety and result in boredom.(10)
Checklists, which can improve safety in the operating room by reducing failure to perform certain tasks (11,12), would likely not have helped for the repetitive task of verifying that the NIBP cuff is still cycling intermittently. As pointed out in the case report, most patient monitors gray-out stale blood pressure values or at least show their age, and the device also could have alerted the CRNA to the fact that the blood pressure has not been measured for a defined period of time. However, having a "stale blood pressure alert," which might seem like a logical solution, could lead to an increase in alarm fatigue.(13) Also, common situations (1) such as patient position changes, presence of invasive catheters for blood pressure measurement, or wait periods before post-anesthesia care unit transfer might warrant discontinuing constant blood pressure measurements. Hence, a stale blood pressure alert would likely decrease patient safety instead of improving it. If the patient monitor had simply stopped displaying the stale blood pressure value, it would be more likely to draw the CRNA's attention. Finally, if there was no simple indication by the patient monitor that the NIBP cuff wasn't cycled for a period of time, it should be removed from service in this location to prevent this error from reoccurring.
Another approach to preventing this error would be to use the electronic anesthesia record to identify the problem. Decision support features within the anesthesia record could alert providers that neither NIBP cuff blood pressure measurements nor alternate measurements (such as from an arterial line) are currently being obtained.(14) In the presented scenario, such decision support may have led to better situational awareness and helped clinicians identify this patient's problem earlier. This is merely one of a number of potential opportunities for decision support within an anesthesia information management system, such as detecting drug overdose based on hemodynamic responses (15), antibiotic administration compliance, and postoperative nausea and vomiting prophylaxis.(16) However, using an electronic anesthesia record by itself is not without problems, as failure to detect loss of connectivity between the patient monitor and electronic anesthesia record system has led to litigation.(17)
In the presented case, a simple reminder ("check if NIBP is cycling—value not grayed out as in main OR") might have been sufficient to prevent this event—pointing out the difference between this patient monitor's behavior and the commonly used patient monitors in the core operating room with respect to blood pressure measurement. Additional training to familiarize providers with the equipment used in the catheterization laboratory or magnetic resonance imaging scanner is especially important, due to the remoteness of the procedure location and lack of direct supervision and/or immediately available help, and should be considered before allowing practice in these settings, as well as periodic updates. Finally, a decision support alert from the electronic anesthesia record would likely have prevented this error from occurring in the first place.
Take-Home Points
- Anesthesia machines and patient monitors commonly differ between the non-operating room and core operating room settings. Familiarity with these devices and emergency equipment is of great importance in these remote settings as help or support may be less available. Harmonized monitor design within a hospital would alleviate this risk.
- Older devices with less safety enhancements are often relegated to non-operating room settings. This may pose safety hazards.
- Interruptions in blood pressure measurements from the NIBP cuff frequently occur during anesthesia and can be reduced by optimized monitor design or using reminders from an anesthesia information system.
- Electronic anesthesia records capture more relevant clinical data, contain less "smoothing" of documented vital signs, and allow the use of decision support systems to alert anesthesia providers of potential problems while providing solutions for consideration.
Matthias Görges, PhD Post-Doctoral Fellow University of British Columbia Pediatric Anesthesia Research Team (PART) Vancouver, BC, Canada
J. Mark Ansermino, MBBCh, MSc Senior Associate Clinician Scientist, CFRI Director, Innovations in Acute Care & Technology research cluster, CFRI Associate Professor, Department of Anesthesia, University of British Columbia Director of Research for Pediatric Anesthesia, BC Children's Hospital Vancouver, BC, Canada
References
1. Ehrenfeld JM, Epstein RH, Bader S, Kheterpal S, Sandberg WS. Automatic notifications mediated by anesthesia information management systems reduce the frequency of prolonged gaps in blood pressure documentation. Anesth Analg. 2011;113:356-363. [go to PubMed]
2. Gaba DM, Howard SK, Small SD. Situation awareness in anesthesiology. Hum Factors. 1995;37:20-31. [go to PubMed]
3. van Schalkwyk JM, Lowes D, Frampton C, Merry AF. Does manual anaesthetic record capture remove clinically important data? Br J Anaesth. 2011;107:546-552. [go to PubMed]
4. Standards For Basic Anesthetic Monitoring. Schaumburg, IL: American Society of Anesthesiologists Committee on Standards and Practice Parameters; 2011:3.
5. Statement On Nonoperating Room Anesthetizing Locations. Schaumburg, IL: American Society of Anesthesiologists Committee on Standards and Practice Parameters; 2013:2.
6. Metzner J, Posner KL, Domino KB. The risk and safety of anesthesia at remote locations: the US closed claims analysis. Curr Opin Anaesthesiol. 2009;22:502-508. [go to PubMed]
7. Van De Velde M, Kuypers M, Teunkens A, Devroe S. Risk and safety of anesthesia outside the operating room. Minerva Anestesiol. 2009;75:345-348. [go to PubMed]
8. Cooper JB, Newbower RS, Long CD, McPeek B. Preventable anesthesia mishaps: a study of human factors. Anesthesiology. 1978;49:399-406. [go to PubMed]
9. Cassidy CJ, Smith A, Arnot-Smith J. Critical incident reports concerning anaesthetic equipment: analysis of the UK National Reporting and Learning System (NRLS) data from 2006–2008. Anaesthesia. 2011;66:879-888. [go to PubMed]
10. Weinger MB. Anesthesia equipment and human error. J Clin Monit Comput. 1999;15:319-323. [go to PubMed]
11. Hagerman NS, Varughese AM, Kurth CD. Quality and safety in pediatric anesthesia: how can guidelines, checklists, and initiatives improve the outcome? Curr Opin Anaesthesiol. 2014;27:323-329. [go to PubMed]
12. Low D, Walker I, Heitmiller ES, Kurth D. Implementing checklists in the operating room. Paediatr Anaesth. 2012;22:1025-1031. [go to PubMed]
13. Schmid F, Goepfert MS, Kuhnt D, et al. The wolf is crying in the operating room: patient monitor and anesthesia workstation alarming patterns during cardiac surgery. Anesth Analg. 2011;112:78-83. [go to PubMed]
14. Nair BG, Horibe M, Newman SF, Wu WY, Schwid HA. Near real-time notification of gaps in cuff blood pressure recordings for improved patient monitoring. J Clin Monit Comput. 2013;27:265-271. [go to PubMed]
15. Nair BG, Horibe M, Newman SF, Wu WY, Peterson GN, Schwid HA. Anesthesia information management system-based near real-time decision support to manage intraoperative hypotension and hypertension. Anesth Analg. 2014;118:206-214. [go to PubMed]
16. Rothman B, Leonard JC, Vigoda MM. Future of electronic health records: implications for decision support. Mt Sinai J Med. 2012;79:757-768. [go to PubMed]
17. Vigoda MM, Lubarsky DA. Failure to recognize loss of incoming data in an anesthesia record-keeping system may have increased medical liability. Anesth Analg. 2006;102:1798-1802. [go to PubMed]
18. Liu D, Görges M, Jenkins SA. University of Queensland vital signs dataset: development of an accessible repository of anesthesia patient monitoring data for research. Anesth Analg. 2012;114:584-589. [go to PubMed]
Figure
Figure: Example of an anesthetic record showing NIBP measurements missing for approximately 15 minutes.(18)