An Ounce of Prevention
Case Objectives
- Assess risk for venous thromboembolism (VTE) in hospitalized patients
- List recommended strategies for VTE prevention for various risk groups
- Identify patients who qualify for extended-duration prophylaxis
- Appreciate interventions that may increase system-wide use of VTE prophylaxis
Case & Commentary: Part 1
A 47-year-old woman was admitted to the plastic surgery service after a motor vehicle collision with major trauma to her right hand, which required repair with use of an abdominal flap. On the second postoperative day, the patient suffered a sudden cardiopulmonary arrest. After successful resuscitation, a chest CT revealed a massive pulmonary embolism.
Venous thromboembolism (VTE) is a common condition, with an incidence of 1.5/1000 per year in all U.S. adults and at least 1% of hospitalized patients.(1) Deep vein thrombosis (DVT) is associated with a 30-day mortality rate of less than 2% (in fact, many cases go undiagnosed and undetected), but pulmonary embolism (PE) is far more serious, with an overall 30-day mortality of approximately 10%.(2) Most early PE deaths are due to acute right ventricular failure, whereas late PE mortality often is caused by the underlying conditions that predisposed to the clot. In the United States, more than 100,000 patients per year die from PE.(3)
The most common VTE risk factors include surgery, trauma, cancer, congestive heart failure, chronic lung disease, age older than 70 years, obesity, bed rest, prior VTE, thrombophilic disorders, and acute respiratory failure. Recurrences are common: more than 50% of surgical patients with a previous history of VTE who do not receive prophylaxis will develop postoperative DVT.(4) Nearly one in five surgeries (even in the absence of additional risk factors) results in VTE if neither pharmacologic nor mechanical prophylaxis is applied.(5) That number skyrockets to more than 50% in patients undergoing total hip and total knee replacement who fail to receive prophylaxis.(6) Spinal surgery, pelvic surgery, and neurosurgery also place patients at particularly high risk of VTE.
Trauma, particularly of the lower extremities and pelvis, increases the risk of VTE. PE has been identified at autopsy in as many as 60% of patients with lower-extremity fractures (7), and mortality has been attributed to PE in as many as 50% of patients dying after hip fracture.(8) The incidence of VTE increases with time after the traumatic event. Autopsy-confirmed PE in patients surviving less than 24 hours after trauma has been demonstrated in 3.3%, increasing to 5.5% in those surviving up to 7 days. PE was found in 18.6% of those surviving a longer period.(9) The risk of VTE after major trauma to the upper extremity is less clear. In this setting, lower-extremity DVT often is caused by prolonged bed rest; the risk increases when surgery and general anesthesia are required. Upper-extremity trauma enhances the risk of upper-extremity DVT.(10) The risk of symptomatic PE in patients with lower-extremity DVT ranges between 15% and 30% (11), and it occurs less often (3%) in patients with upper-extremity DVT.(10)
Case & Commentary: Part 2
Review of the patient's chart revealed no pre- or postoperative DVT prophylaxis.
Without knowing the full extent of this patient’s trauma and the presence of additional risk factors, it is impossible to say if prophylaxis should have been administered. The critical point for clinicians is to consider this risk and make appropriate, evidence-based decisions about prophylaxis in all hospitalized patients.
Despite detailed North American guidelines, VTE prophylaxis continues to be underutilized. In a registry of 5,451 consecutive patients with ultrasound-confirmed DVT from 183 United States institutions, only 42% of inpatients had received prophylaxis within 30 days prior to developing acute DVT.(12) In this registry, compliance with guidelines was better in surgical than in medical patients.
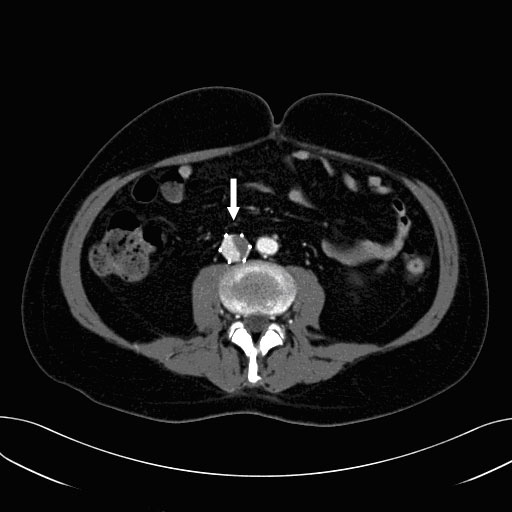
VTE prophylaxis recommendations differ for the various surgical settings (Table). According to current consensus guidelines from the American College of Chest Physicians (ACCP) (13), prophylaxis should be administered in all trauma patients with at least one additional risk factor. Low-molecular-weight heparin (LMWH) is recommended as pharmacologic prophylaxis. In some patients, however, the use of LMWH may be precluded, usually because of the risk of bleeding. In such patients, mechanical prophylaxis, including graduated compression stockings or intermittent pneumatic compression devices, should be considered. Ultrasound surveillance, seeking evidence of DVT that would tip the scales toward anticoagulation (or, if that is too risky, placement of an inferior vena cava [IVC] filter), is recommended in high-risk trauma patients not receiving pharmacologic prophylaxis. The ACCP recommends against the routine (ie, prophylactic) use of IVC filters in trauma patients. Newer retrievable IVC filters may be useful for patients with transiently increased risk of both clotting and bleeding complications, and many institutions now use them in this setting. Although permanent IVC filters reduce the risk of PE, there is a tradeoff: the risk of DVT at 1 year, particularly due to filter thrombosis (Figure 1), is double that of patients without filters.(14)
Case & Commentary: Part 3
The patient was aggressively resuscitated and started on systemic anticoagulation with heparin, and then warfarin. After a 3-day stay in the intensive care unit, the patient was transferred to the floor. Ultimately, she was discharged to home without any evidence of anoxic brain injury or permanent pulmonary sequelae from her PE.
In 2003, the American Public Health Association (APHA) created a national coalition to advocate for greater awareness of DVT and PE among health care providers and the general public.(15) The Joint Commission on Accreditation of Healthcare Organizations (JCAHO) has been encouraged by the APHA to make adherence to DVT prevention guidelines part of its accreditation process. As of now, specific actions from JCAHO have not been undertaken, and DVT prophylaxis still is not part of ratings for hospital performance.
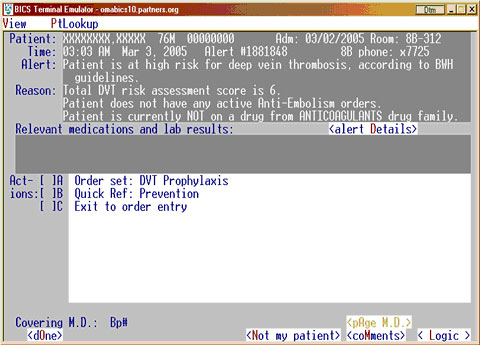
Continuing medical education (16) and computerized electronic alerts (17,18) can increase physician utilization of VTE prophylaxis. In a randomized controlled trial of 2506 high-risk patients who did not receive prophylaxis, a single computer alert to the responsible physician doubled the prophylaxis rate and reduced the VTE rate at 90 days by 41%.(19) The computer program used eight common risk factors to determine each hospitalized patient's risk profile for VTE on a daily basis. Each risk factor was weighted according to a point scale: the major risk factors of cancer, prior VTE, and hypercoagulability were assigned a score of 3; the intermediate risk factor of major surgery was assigned a score of 2; and the minor risk factors of advanced age, obesity, bed rest, and the use of hormone-replacement therapy or oral contraceptives were assigned a score of 1. An increased risk of VTE was defined as a cumulative risk score of at least 4. In patients with a VTE risk score greater than or equal to 4, the computer program used medical record numbers to randomly assign 1255 eligible patients to an intervention group, in which the responsible physician was alerted to a patient's risk of DVT, and 1251 patients to a control group, in which no alert was issued. The alert was sent once for each patient (Figure 2). The physician was required to acknowledge the alert and could then withhold or order prophylaxis, including graduated compression stockings, pneumatic compression boots, unfractionated heparin, LMWH, or warfarin. The results of this trial suggest that hospitals with adequate information system resources should consider implementation of electronic alerts to increase the awareness of VTE risk, to improve the utilization of prophylaxis, and to reduce the rates of DVT and PE.
Take-Home Points
- Know the common VTE risk factors.
- Assess VTE risk for each hospitalized patient individually.
- Become familiar with the various VTE prophylaxis regimens for different patient groups at risk.
- Apply the current ACCP guidelines to prevent VTE in hospitalized patients.
- Use hospital information systems to increase awareness of VTE and implement adequate prophylaxis in patients at risk.
Nils Kucher, MD Staff Interventional Cardiologist Department of Medicine, Cardiovascular Division University Hospital Zurich Switzerland
Faculty Disclosure: Dr. Kucher has declared that neither he, nor any immediate member of his family, has a financial arrangement or other relationship with the manufacturers of any commercial products discussed in this continuing medical education activity. In addition, his commentary does not include information regarding investigational or off-label use of pharmaceutical products or medical devices.
References
1. Tsai AW, Cushman M, Rosamond WD, Heckbert SR, Polak JF, Folsom AR. Cardiovascular risk factors and venous thromboembolism incidence: the longitudinal investigation of thromboembolism etiology. Arch Intern Med. 2002;162:1182-1189. [ go to PubMed ]
2. Goldhaber SZ, Visani L, De Rosa M. Acute pulmonary embolism: clinical outcomes in the International Cooperative Pulmonary Embolism Registry (ICOPER). Lancet. 1999;353:1386-1389. [ go to PubMed ]
3. Goldhaber SZ. Pulmonary embolism. Lancet. 2004;363:1295-1305. [ go to PubMed ]
4. Kakkar VV, Howe CT, Nicolaides AN, Renney JT, Clarke MB. Deep vein thrombosis of the leg: Is there a "high risk" group? Am J Surg. 1970;120:527-530. [ go to PubMed ]
5. Clagett GP, Reisch JS. Prevention of venous thromboembolism in general surgical patients: results of meta-analysis. Ann Surg. 1988;208:227-240. [ go to PubMed ]
6. Clagett GP, Anderson FA Jr, Geerts W, et al. Prevention of venous thromboembolism. Chest. 1998;114(suppl 5):531S-560S. [ go to PubMed ]
7. Fisher M, Michele A, McCann W. Thrombophlebitis and pulmonary infarction associated with fractured hip. Clin Res. 1963;11:407.
8. Fitts, WT Jr, Lehr HB, Bitner RL, Spellman JW. An analysis of 950 fatal injuries. Surgery. 1964;56:663-668. [ go to PubMed ]
9. Coon WW. Risk factors in pulmonary embolism. Surg Gynecol Obstet. 1976;143:385-390. [ go to PubMed ]
10. Joffe HV, Kucher N, Tapson VF, Goldhaber SZ, for the Deep Vein Thrombosis (DVT) FREE Steering Committee. Upper-extremity deep vein thrombosis: a prospective registry of 592 patients. Circulation. 2004;110:1605-1611. [ go to PubMed ]
11. Kucher N, Tapson VF, Goldhaber SZ, for the DVT FREE Steering Committee. Risk factors associated with symptomatic pulmonary embolism in a large cohort of DVT patients. Thromb Haemost. 2005;93:494-498. [ go to PubMed ]
12. Goldhaber SZ, Tapson VF, for the DVT FREE Steering Committee. A prospective registry of 5,451 patients with ultrasound-confirmed deep vein thrombosis. Am J Cardiol. 2004;93:259-262. [ go to PubMed ]
13. Geerts WH, Pineo GF, Heit JA, et al. Prevention of venous thromboembolism: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest. 2004;126(suppl 3):338S-400S. [ go to PubMed ]
14. Decousus H, Leizorovicz A, Parent F, et al, for the Prévention du Risque d'Embolie Pulmonaire par Interruption Cave Study Group. A clinical trial of vena caval filters in the prevention of pulmonary embolism in patients with proximal deep-vein thrombosis. N Engl J Med. 1998;338:409-415. [ go to PubMed ]
15. Public Health Leadership Conference on Deep-Vein Thrombosis. Deep-vein thrombosis: advancing awareness to protect patient lives. Washington, DC: American Public Health Association; 2003. Available at: http://www.apha.org/ppp/DVT_White_Paper.pdf. Accessed December 13, 2005.
16. Anderson FA Jr, Wheeler HB, Goldberg RJ, Hosmer DW, Forcier A, Patwardhan NA. Changing clinical practice. Prospective study of the impact of continuing medical education and quality assurance programs on use of prophylaxis for venous thromboembolism. Arch Intern Med. 1994;154:669-677. [ go to PubMed ]
17. Dexter PR, Perkins S, Overhage JM, Maharry K, Kohler RB, McDonald CJ. A computerized reminder system to increase the use of preventive care for hospitalized patients. N Engl J Med. 2001;345:965-970. [ go to PubMed ]
18. Durieux P, Nizard R, Ravaud P, Mounier N, Lepage E. A clinical decision support system for prevention of venous thromboembolism: effect on physician behavior. JAMA. 2000;283:2816-2821. [ go to PubMed ]
19. Kucher N, Koo S, Quiroz R, et al. Electronic alerts to prevent venous thromboembolism among hospitalized patients. N Engl J Med. 2005;352:969-977. [ go to PubMed ]
Table
Table. VTE Prophylaxis Modalities for Common Surgical Settings
| Indication | Prevention Strategy |
|---|---|
| General surgery | UFH 5,000 units q 8h, 1st dose 2h preoperatively, continued for 7 days or LMWH once daily. |
| Cancer surgery | Enoxaparin 40 mg daily, 1st dose 10-14h preoperatively if possible, for 28 days. |
| Total hip replacement | Enoxaparin 40 mg daily, beginning preoperative evening, continuing out-of-hospital for 21-28 days. |
| Enoxaparin 30 mg BID, 1st dose 12-24h postoperatively, until hospital discharge. | |
| Dalteparin 2,500 units ≥ postoperatively, then 5,000 units daily until hospital discharge or for 35 days. | |
| Fondaparinux 2.5 mg 4-8h postoperatively, then ≥ 12h after 1st dose, then daily for 5-9 days. | |
| Warfarin daily, 1st dose 7.5 mg 24-48h preoperatively, adjusted to target INR of 2.0-3.0. | |
| Warfarin daily, 1st dose 5 mg preoperative evening, adjusted to target INR of 2.0-3.0 and continued 4-6 weeks. | |
| Total knee replacement | Enoxaparin 30 mg BID, beginning 12-24h postoperatively, continued for an average of 9 days. |
| Fondaparinux 2.5 mg, 1st dose 4-8h postoperatively, 2nd dose ≥ 12h after 1st dose, then daily for 5-9 days. | |
| Hip fracture surgery | Fondaparinux 2.5 mg, 1st dose 4-8h postoperatively, 2nd dose ≥ 12h after 1st dose, then daily for 5-9 days. If surgery is delayed > 24-48h after admission, give 1st dose 10-14h preoperatively. Continue prophylaxis for 28-35 days after surgery. |
| Neurosurgery | Enoxaparin 40 mg daily, 1st dose ≤ 24h postoperatively, continued until hospital discharge, plus GCS. |
| Craniotomy for brain tumor | Enoxaparin 40 mg daily or UFH 5,000 units BID, 1st dose on 1st postoperative morning, continued until hospital discharge, plus GCS/IPC, plus predischarge venous ultrasonography. |
| UFH = unfractionated heparin, LMWH = low-molecular-weight heparin, GCS = graduated compression stockings, IPC = intermittent pneumatic compression devices | |
Figures
Figure 1. CT Scan in a Patient with Inferior Vena Cava (IVC) Filter Thrombosis, Causing 50% Obstruction of the IVC
Figure 2. Example Electronic VTE Alert System (Brigham and Women's Hospital)