Triage Time Bomb
The Case
A parent presented with a child to the emergency department (ED) triage area (located around the corner and down the hall from the actual ED). The child was febrile, and had been vomiting and having diarrhea. After evaluating the child, who was still vomiting and had several episodes of diarrhea in the triage cubicle, the triage nurse was unsure about how to administer acetaminophen to the child. The nurse walked back to the ED to ask the physician about this. The doctor advised the nurse to bring the child to an ED exam room immediately (rather than wait for her "turn"), so that the child could be evaluated and receive intravenous (IV) fluid and possibly antiemetics. The physician explained to the nurse that the child might be dehydrated, and that acetaminophen could be given once these symptoms were controlled.
After receiving these instructions from the doctor, the nurse alerted the ED charge nurse of the plan. This nurse told the triage nurse not to bring the child back to the ED yet, because not enough staff members were available to care for the child. She stated that some patients were being discharged, and when they were, then the child could be brought back. The triage nurse walked back out of the ED and down the hallway and relayed this altered plan to the child’s parent, who then decided to take the child elsewhere for treatment.
Later in the evening, it was discovered that the child had been taken to another local hospital ED in full arrest.
The Commentary
One of the key tenets of emergency department care is the ability and expectation to provide immediate access and stabilization for patients with medical emergencies. This case illustrates a breakdown in triage and emergency care at multiple levels, as well as the consequences of ED overcrowding.
How common is this scenario?
Emergency department overcrowding is ubiquitous; in a nationwide survey, 91% of ED directors reported that overcrowding is a problem.(1) Common definitions of overcrowding include: patients in hallways, all ED beds occupied, waiting rooms full more than 6 hours per day, and acutely ill patients waiting longer than 60 minutes to see a physician. The causes of overcrowding are multifactorial. A statewide evaluation of waiting times in California EDs found that, not surprisingly, higher ratios of waiting room patients to physicians and triage nurses were associated with longer waits.(2) Increasing patient volume and acuity, hospital bed shortages, nursing shortages, and delays in response time of on-call specialists have also been cited as contributing causes.(1,3)
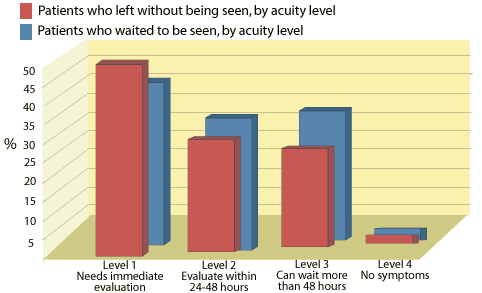
The patient safety issues raised in this case are not uncommon. According to a report from the Centers for Disease Control and Prevention (CDC) report on ED use, in the United States in 2000, 1.8 million patients walked out of EDs without being seen.(4) Increased ED volume and associated long waits for care have been linked to patients leaving prior to physician evaluation and suffering adverse consequences, as in this case. At one large urban public hospital, more than 50% of those who left did so because they felt too sick to continue to wait; 11% of those who left were hospitalized emergently within the next week.(5) However, the patients who left needed medical care just as much as those who stayed (Figure). The United States Office of Inspector General and the Health Care Financing Administration note that a hospital may violate the patient antidumping statute if it routinely keeps patients waiting so long that they leave without being seen.(6) This is particularly true if the hospital does not attempt to determine and document why individual patients are leaving, and reiterate to them that the hospital is prepared to provide medical screening if they stay. In this case scenario, the message relayed to the child's parents was that the hospital was not currently prepared to provide timely care.
What is the purpose of emergency department triage?
Triage processes have evolved as one way to manage a growing patient volume that is beyond the ED's capacity to provide immediate care for all. Triage, derived from the French verb trier, meaning to sort or to choose, is the process by which patients are sorted or prioritized according to the type and urgency of their conditions. Originating on the battlefields of World War I, the triage process emerged in hospitals in the late 1950s and early 1960s in response to increasing volume and use of EDs. The goals of triage are to promptly identify patients requiring immediate treatment of life-threatening conditions, and "sort" or prioritize for care other patients according to their acuity. Standards of practice in emergency nursing and medicine suggest maximum acceptable waiting times for care based on patient acuity level. Since acuity level is not necessarily static, patients in the waiting area need periodic reassessments to assure that their conditions do not warrant more immediate care. EDs should develop protocols to facilitate this process.
How reliable is ED triage?
Despite widespread use for decision-making in prioritizing patient care, current triage methods are limited in reliability and accuracy. As in this scenario, nurses often conduct ED triage by using their clinical judgment and experience in the absence of written guidelines or other aids. Implicit criteria used by triage nurses to classify patients vary from hospital to hospital, shift to shift, and even nurse to nurse.(7) A national cross-sectional evaluation of hospital EDs found incorrect triage rates of 5.5%.(7) High mis-triage rates are attributable to lack of standardization and validation of triage processes.(8) Implementation of explicit standardized screening guidelines has been demonstrated to improve reliability and safety of ED screening.(9-12) In a comparison of ED physician, nurse, and computer-assisted triage, computer-assisted triage was the most sensitive in identifying patients who subsequently required hospitalization.(8) On the other hand, physicians were more specific in identifying those who did not.
Should triage decisions change when the emergency department is overcrowded?
The triage nurse in this scenario did not recognize the acuity of the child's condition. Staffing triage areas with experienced ED nurses or physicians, and incorporating written protocols can reduce this type of error. After consultation with the ED physician, the patient's acuity level was upgraded to one that required immediate care. The charge nurse erred when she told the triage nurse not to bring the patient into the treatment area. Decisions regarding the safe timing of care should not change when an ED is overcrowded. An ED waiting area is not appropriately staffed or equipped to monitor unstable patients, making even an overcrowded treatment area the better choice. The decision of the charge nurse may have represented a failure of communication between the two nurses as well. The response of many EDs to this mismatch of patient volume, acuity, and available beds is to move patients awaiting discharge out of ED beds, and divert ambulance traffic until additional high acuity patients may be accommodated. Unfortunately, ambulance diversion may have a domino effect, increasing overcrowding at neighboring EDs.
What should be the response of EDs to overcrowding?
The Crowding Resources Task Force of the American College of Emergency Physicians developed recommendations for short- and long-term solutions to ED overcrowding.(13) At the emergency department level, best practices to address overcrowding include: real-time monitoring of ED crowding metrics with the goal to identify problems before they get out of control; using written triage protocols; having flexible ED and triage staffing that allow for adjustment of staffing as needed; automating processes where possible (eg, using patient tracking software); and expanding fast-track and observation services.
In the end, of course, these measures must be placed in the context of the broader health care environment. The systemic problems that lead to ED overcrowding (such as the nursing shortage and the barriers to primary care for some patients) must also be addressed. Otherwise, even EDs that thoughtfully implement triage strategies and protocols are likely to be overwhelmed by the magnitude of their task too often.
Take-Home Points
- Implementation of explicit standardized ED screening guidelines can improve reliability and safety of ED screening.
- Periodic reassessments of patients awaiting ED care are necessary to detect any changes in their acuity level.
- Decisions regarding the timing of care should not change when an ED is overcrowded.
- EDs should have protocols in place for safe delivery of patient care under overcrowded conditions.
Donna L. Washington, MD, MPH Associate Professor of Medicine VA Greater Los Angeles Healthcare System University of California, Los Angeles
References
1. Derlet RW, Richards JR, Kravitz RL. Frequent overcrowding in U.S. emergency departments. Acad Emerg Med. 2001;8:151-5.[ go to PubMed ]
2. Lambe S, Washington DL, Fink A, et al. Waiting times and capacity in California's emergency departments. Ann Emerg Med. 2003 Jan;41:35-44.[ go to PubMed ]
3. Lambe S, Washington DL, Fink A, et al. Trends in the use and capacity of California’s emergency departments, 1990-1999. Ann Emerg Med. 2002;39:389-96.[ go to PubMed ]
4. McCaig LF, Ly N. National hospital ambulatory medical care survey: 2000 emergency department summary. Hyattsville, MD: National Center for Health Statistics; 2002. Advance data from vital and health statistics, No. 326. Available at: [ go to related site ]
5. Baker DW, Stevens CD, Brook RH. Patients who leave a public hospital emergency department without being seen by a physician. Causes and consequences. JAMA. 1991;266:1085-90.[ go to PubMed ]
6. Brown JG, Hash MM. OIG/HCFA special advisory bulletin on the patient anti-dumping statute. Office of Inspector General and Health Care Financing Administration; November 10, 1999. Vol. 64, No. 217. Available at: [ go to related site ]
7. Young GP, Wagner MB, Kellermann AL, Ellis J, Bouley D. Ambulatory visits to hospital emergency departments. Patterns and reasons for use. 24 Hours in the ED Study Group. JAMA. 1996;276:460-5.[ go to PubMed ]
8. Brillman JC, Doezema D, Tandberg D, et al. Triage: limitations in predicting need for emergent care and hospital admission. Ann Emerg Med. 1996;27:493-500. Washington DL, Shekelle PG, Stevens CD. Deferred care for adults with musculoskeletal complaints. Eff Clin Pract. 2001;4:65-72.[ go to PubMed ]
9. Washington DL, Shekelle PG, Stevens CD. Deferred care for adults with musculoskeletal complaints. Eff Clin Pract. 2001;4:65-72.[ go to PubMed ]
10. Washington DL, Stevens CD, Shekelle PG, Baker DW, Fink A, Brook RH. Safely directing patients to appropriate levels of care: guideline-driven triage in the emergency service. Ann Emerg Med. 2000;36:15-22.[ go to PubMed ]
11. Washington DL, Stevens CD, Shekelle PG, Henneman PL, Brook RH. Next-day care for emergency department users with nonacute conditions. A randomized, controlled trial. Ann Intern Med. 2002;137:707-14.[ go to PubMed ]
12. Berman DA, Coleridge ST, McMurry TA. Computerized algorithm-directed triage in the emergency department. Ann Emerg Med. 1989;18:141-4.[ go to PubMed ] Accessed October 23, 2003.
13. Crowding Resources Task Force. American College of Emergency Physicians. Responding to emergency department crowding: a guidebook for chapters; 2002. Accessed October 23, 2003.
Figure
Figure. Percentage of ED patients (by acuity level) who left without being seen and those who waited. No significant differences were detected in how urgently patients needed medical attention. (5)