Nosy Business
The Case
A 59-year-old man with a history of idiopathic thrombocytopenic purpura (ITP) presented to the emergency department (ED) with epistaxis (a "nose bleed"). He reported no previous history of epistaxis and stated that the symptoms began spontaneously a few hours prior to presentation. He was treated with "conservative" therapy after his platelet count was found to be normal and discharged home. He returned to the ED 24 hours later with recurrence of epistaxis and was once again discharged home after the bleeding stopped spontaneously. When he presented with epistaxis for the third time in 72 hours, he was noted to be tachycardic and pale. He had developed a new anemia, but his platelet count remained normal and his tachycardia resolved with intravenous fluids.
The ED providers initially placed nasal tampons bilaterally, but his brisk bleeding continued. Otolaryngology was consulted and, after removing the tampons, they identified the posterior nasopharynx as the site of bleeding under direct visualization. After attempted cautery and nasal packing, the bleeding recurred within an hour. The patient ultimately underwent a procedure to have his sphenopalatine artery embolized by interventional radiology. Because the patient's platelet count remained normal through the bleeding episodes, a hematology consultant felt that the patient's ITP had not contributed to the epistaxis. The patient's symptoms resolved, he received 4 units of packed red blood cells, and he was discharged home with no immediate recurrence.
The Commentary
Nearly all of us have experienced a simple nose bleed. They are frequently minor and self-limited, occur more commonly in children and adolescents, and often result from local trauma, including self-induced "digital trauma." However, as this case demonstrates, epistaxis can be severe, requiring transfusion, angiographic or surgical intervention, and inpatient intensive care. Most severe nose bleeds of this nature occur in individuals older than 50 years.(1)
Anatomy & Epidemiology
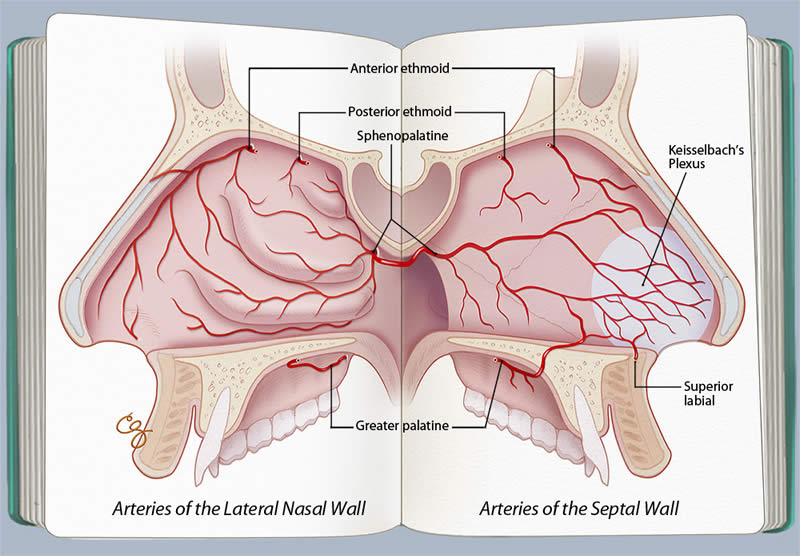
Functionally speaking, the nose processes thousands of liters of air per day, trapping irritants and humidifying the air before it enters the lungs. The anterior nasal cavity is therefore subject to drying and inflammation, making it more prone to occasional bleeding. Epistaxis results from both local and systemic etiologies.(1-3) Common local factors include digital trauma, nasal septal deviation, nasal cannula oxygen, and intranasal corticosteroid use. Underlying clotting disorders, renal failure, and alcoholism are common systemic factors. Neoplasm is a rare cause but should be considered in individuals with recurring bleeds from the same side, particularly when accompanied by nasal obstruction.(4) The nasal cavity is richly vascular and supplied with multiple arteries that provide opportunities for epistaxis in the right setting. Just inside the nostril and along the midline septum is an area where these arterial supplies meet, commonly referred to as Kiesselbach's plexus or triangle. This area is the most common location of epistaxis. The vast majority of nose bleeds originate from this area, but the less frequent and more serious bleeds can arise from deeper within the nose. Epistaxis is therefore often operationally divided into "anterior" and "posterior" epistaxis. In other words, bleeds controlled with simple anterior packing or cautery are classified as anterior and those requiring posterior packing or more invasive procedures are defined as posterior. Anterior epistaxis typically arises from the anterior ethmoidal artery or superior labial artery circulation while posterior epistaxis arises from the sphenopalatine or posterior ethmoid arteries (Figure). Posterior bleeds are more commonly seen in older individuals, and their management is more complex, typically requiring the involvement of an otolaryngologist.
Home Management
Epistaxis is typically managed at home without specific medical intervention. Similar to bleeding from other sites, it is most effectively controlled by direct pressure. Pinching the nostrils together puts direct pressure on Kiesselbach's plexus and can slow or stop the bleeding. Pinching the upper lip "pressure point" also diminishes blood coming in from the upper lip artery. Tilting the head forward allows blood to intermittently leave the nose, although a more supine or recumbent position may be more comfortable for patients who feel lightheaded. Any blood leaving the nasal cavity and flowing posteriorly into the pharynx should be spit out, as blood that is swallowed and enters the stomach can provoke nausea. Placing wads of facial tissue or other items into the nose beyond the skin-lined vestibule should be discouraged, as these items typically cause further trauma to the nasal mucosa, possibly worsening the bleeding.
Medical Management
When bleeding either fails to respond to the above measures or is profuse, patients should seek medical treatment in an urgent or emergency care setting. Providers should always begin with a brief clinical assessment to confirm hemodynamic stability and airway patency. They should then obtain a directed history of the current episode as well as assess the patient for underlying systemic risk factors. If the bleeding has been prolonged, recurrent, or severe, a high index of suspicion for anemia and volume depletion should be present. The amount of blood that can be lost through the nose is frequently underestimated; the providers in this case may well have succumbed to this pitfall during the patient's first two encounters.
Following immediate stabilization of the patient's hemodynamics and ensuring a protected airway, the next key step is precisely identifying the source of the bleeding to allow for an accurate and effective treatment plan. Topical vasoconstrictors are often effective in slowing, if not stopping, bleeding from the anterior septum. They are often administered with a topical anesthetic to facilitate the examination. A strong light source and suction for removing blood and clots are essential for identifying the bleeding source, although care must be taken to avoid injuring the mucosa with suctioning. Not only do these injuries create additional bleeding sources, they are commonly mistaken for the original source, preventing its proper identification. When no source can be identified anteriorly, nasal endoscopy should be considered. Nasal endoscopy can be performed by the primary care physician or emergency care provider trained in its use, but is often performed by an otolaryngologist.
Once the source of the bleeding has been identified, cauterization, either chemical with silver nitrate sticks (Video) or electrical with a monopolar or bipolar device, targets the bleeding site and is quite effective. Because it devascularizes the septal mucosa locally, cauterization should be limited to one side of the nasal septum to avoid a septal perforation.(5) Moisturizing the nasal cavity is important while the cautery wound heals to avoid recurrence of the bleeding but, if necessary, the cautery can be repeated.
Packing has traditionally been used for epistaxis, but it in some sense can resemble a sledgehammer being used to attack a fine nail. Precisely identifying the source allows for targeted treatment that may obviate traditional nasal packing, even in the patient with an underlying bleeding disorder. In certain patients, the source cannot be identified or the bleeding is diffuse, which is more often than not due to trauma from the examination rather than the original bleeding. In these cases, packing is a reasonable solution. However, it must be noted that packing is very uncomfortable for patients, and its removal is often associated with additional bleeding due to disruption of clots (6,7), particularly in the coagulopathic patient. Traditional packs, including balloons and petroleum jelly–impregnated gauze, are beginning to give way to newer biomaterials that are resorbable, obviating the need for removal.(4) A prospective randomized controlled study showed that, for initial ED control of epistaxis, absorbable biomaterials are easier to use, less painful, and more effective than traditional packing.(8) While initially more expensive than traditional packing, these materials may render otolaryngology consultation and/or subsequent packing removal unnecessary.
When anterior cautery and packing fail, the most likely source of the bleeding is far posterior within the nasal cavity. Again, the definition of anterior versus posterior epistaxis is pragmatically an operational one. Posterior epistaxis warrants an otolaryngology consultation as the less accessible source of the bleed typically requires more specialized procedures. These cases of posterior epistaxis can be temporized by packing the nasopharynx and posterior nasal cavity, but often require surgical cautery or ligation of the sphenopalatine artery or angiographic embolization. Both modalities are effective, but surgical intervention may be more cost effective.(9)
Summary
This case reinforces a number of important points about managing patients with epistaxis. First, the bleeding source must be accurately identified and treated. Epistaxis often stops spontaneously, only to recur unexpectedly within hours or days. Identifying the bleeding source, even if this means disrupting a clot within the nose, allows cauterization or focal biomaterial application and may prevent frequent returns to the emergency department, as occurred with this patient. While "conservative" management is in the eye of the beholder, it appears unlikely that the bleeding source in this patient was sought or accurately identified until his third visit and after significant blood loss. A thorough examination with good lighting and suctioning would likely have demonstrated a posterior source, prompting earlier referral to a specialist who could have more effectively treated this patient.
Second, underlying potential coagulopathy does not affect the need to acutely stop the bleeding. Although a patient with an underlying clotting disorder may present with epistaxis, the acute treatment is often not significantly affected by the systemic disorder. In fact, it appears that this patient's ITP was not an aggravating factor in his recurrent epistaxis. Coagulopathies that can be corrected should be, but these are often addressed over the course of hours or days while the bleeding nose needs to be addressed acutely.
Finally, epistaxis patients should be assessed for hemodynamic stability. While many cases of epistaxis are minor, some can be life-threatening emergencies. Frequently recurring, profuse, or prolonged bleeding cases may be associated with significant blood loss. Airway and hemodynamic considerations should not be neglected, even in cases that appear straightforward.
Take-Home Points
- Epistaxis patients should be assessed for hemodynamic stability and airway protection, as the amount of blood loss is often underestimated.
- The specific bleeding source should be precisely identified as this allows for appropriate and targeted therapy. It is particularly crucial to separate anterior versus posterior sources; the latter usually require specialized expertise to address effectively.
- While an underlying or potential coagulopathy needs to be addressed, it generally does not alter the acute management, which focuses on hemodynamics and controlling the local bleeding source.
Richard R. Orlandi, MD Associate Professor
Otolaryngology, Head and Neck Surgery
The University of Utah
References
1. Massick D, Tobin EJ. Epistaxis. In: Cummings CW, Haughey BH, Thomas JR, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. Philadelphia, PA: Mosby, Inc.; 2005. ISBN: 9780323019859.
2. Tan LK, Calhoun KH. Epistaxis. Med Clin North Am. 1999;83:43-56. [go to PubMed]
3. Wormald PJ. Epistaxis. In: Bailey BJ, Johnson JT, Newlands SD, Calhoun KH, Deskin RW, eds. Head and Neck Surgery - Otolaryngology. Philadelphia, PA: Lippincott Williams & Wilkins; 2006. ISBN: 9780781755610.
4. Gifford TO, Orlandi RR. Epistaxis. Otolaryngol Clin North Am. 2008;41:525-536. [go to PubMed]
5. Hanif J, Tasca RA, Frosh A, Ghufoor K, Stirling R. Silver nitrate: histological effects of cautery on epithelial surfaces with varying contact times. Clin Otolaryngol Allied Sci. 2003;28:368-370. [go to PubMed]
6. Tai CJ, Chu CC, Liang SC, et al. Use of patient satisfaction data in a continuous quality improvement program for endoscopic sinus surgery. Otolaryngol Head Neck Surg. 2003;129:210-216. [go to PubMed]
7. Orlandi RR, Lanza DC. Is nasal packing necessary following endoscopic sinus surgery? Laryngoscope. 2004;114:1541-1544. [go to PubMed]
8. Mathiasen RA, Cruz RM. Prospective, randomized, controlled clinical trial of a novel matrix hemostatic sealant in patients with acute anterior epistaxis. Laryngoscope. 2005;115:899-902. [go to PubMed]
9. Miller TR, Stevens ES, Orlandi RR. Economic analysis of the treatment of posterior epistaxis. Am J Rhinol. 2005;19:79-82. [go to PubMed]
Figure
Figure. Arterial supply of the lateral and medial nasal walls. (Illustration © by Chris Gralapp.)
Click on thumbnail for larger view.
Video
Video | Title | Length | View |
1 | Silver nitrate cautery | 0:25 | View Video |