Delirium or Dementia?
Case Objectives
- State the key diagnostic differences between delirium and dementia.
- Describe the Confusion Assessment Method for workup of suspected delirium.
- Explain the risks associated with using physical restraints in geriatric inpatients.
- Describe the initial workup of delirium in a hospitalized patient.
Case & Commentary: Part 1
An 86-year-old woman, admitted with complaints of shortness of breath and cough, was found to have pneumonia. Her past medical history included cataract surgery, hypertension controlled with medications, and type 2 diabetes controlled by diet. She was ambulatory, lived alone, and at baseline completed all activities of daily living independently. According to her daughter, the patient was never disoriented. At admission, the patient appeared mildly dehydrated on physical examination. Her oxygen saturation was 94% on 2 liters oxygen by nasal cannula, and an arterial blood gas showed a normal pCO2 of 40 mmHg. Her daughter requested to spend the night at the bedside but was told she could not stay.
Overnight, the patient was noted to be disoriented by the nursing staff. She began pulling at her intravenous lines and attempting to get out of bed. The covering physician was called and ordered that the patient be placed in four-point restraints.
The following morning, the daughter returned to find her mother in restraints, speaking incoherently and severely short of breath. Upon finding her mother confused, the daughter asked the nurse what had happened and reiterated to the nurse that her mother had never been confused before.
Elderly hospitalized patients frequently develop altered mental status as a complication of their illness. Distinguishing delirium from dementia is a common problem for physicians, particularly those who work in hospitals or long-term care facilities. Up to 25% of geriatric general ward patients and as many as 80% of intensive care unit patients experience delirium during hospitalization.(1) Upon presentation to the emergency department, 26% of geriatric patients meet diagnostic criteria for delirium.(2)
Given the frequency of delirium, all patients should be screened for cognitive functioning at the time of hospital admission. Screening serves two important purposes: to assess for delirium upon admission and to provide a baseline if delirium subsequently develops during the hospitalization.
Delirium in the Hospital
In the inpatient setting, any change in mental status should be considered delirium until proven otherwise. In fact, published guidelines preclude making the diagnosis of dementia in the setting of delirium (3); thus, diagnosis of dementia should be reserved for the outpatient setting. Although it is not mentioned whether formal cognitive screening was performed in this patient, the patient's excellent functional status and the corroborating information obtained from her daughter make it unlikely that the patient suffered from dementia at baseline.
Prediction rules for delirium have been validated in medical (4), and non-cardiac (5) and cardiac surgery (6) patients. While each patient population has unique attributes, there are several common, important factors. First, preexisting cognitive deficits are the strongest risk factor for delirium.(4-6) Patients with higher burden of illness, as measured by Acute Physiology, Age, and Chronic Health Evaluation (APACHE) scores (7,8), or comorbidities (5,6) are at higher risk of delirium. Those with laboratory abnormalities, such as a BUN/creatinine ratio ≥18 (a marker of dehydration), decreased albumin, or abnormal sodium, potassium, or glucose (4-6), are also predisposed to develop delirium. Additionally, patients with preexisting sensory deficits (visual or hearing) are at risk for delirium due to decreased cognitive input. For medical patients, cognitive impairment, acuity of illness, visual changes, and dehydration were combined into a validated prediction rule (Table).(4) This patient's pneumonia and dehydration placed her at moderate risk of delirium, even in the absence of preexisting cognitive or visual impairment.
Delirium poses several risks to the patient. First, a delay in diagnosis and assessment of underlying causative factors can cause the underlying condition to fester, resulting in worse physiological function when delirium is discovered. Patients with the hyperactive and mixed variants of delirium (see below for explanation) are at risk for overmedication (particularly sedation). Delirium amplifies the risks of hospitalization and bedrest in older patients, including malnutrition, deconditioning, dehydration, iatrogenic infection (such as catheter-associated urinary tract infection or aspiration pneumonia), pressure ulcers, falls, and iatrogenic events.(9-11) On a larger scale, delirious patients require more staff time (12), resulting in less staff time for other patients.
As a result of all of these factors, delirium is associated with severe consequences for patients. In fact, the diagnosis of delirium carries a mortality risk equivalent to that of sepsis or an in-hospital acute myocardial infarction.(11) Patients who develop delirium have longer length of stay, increased hospital costs, and increased post-hospitalization costs.(13,14) In a recent analysis, patients who developed delirium accrued $16,000 to $64,000 in additional medical costs over the year following hospitalization compared to age-, gender-, and comorbidity-matched controls.(15)
There are three psychomotor variants of delirium: hyperactive (prevalence, 25%), hypoactive (prevalence, 50%), and mixed disorder, with features of both (prevalence, 25%).(16) This patient appeared to have the hyperactive form of delirium. As mentioned above, patients with the hyperactive and mixed disorders are more likely to be physically and chemically restrained. Indeed, this patient was placed in physical restraints when she became confused and hyperactive. The Joint Commission has published standards for restraint use. The key elements of the standards' implementation are "the device's intended use (such as physical restriction), its involuntary application, and/or the identified patient need that determines whether use of the device triggers the application of these standards."(17) As such, consideration should be given to the following questions prior to restraining a patient:
- What is the intended effect of the restraint?
- Is there another means by which the intended effect can be achieved?
- Is this the least invasive restraint?
- Is the use of restraints in the patient's best interest?
- Am I restraining the patient for secondary benefits (to limit phone calls/pages, to assuage nursing requests, too busy to see patient, etc.)?
- When is the restraint going to be removed?
Although necessary at times, the use of restraints must be considered carefully prior to application for three key reasons. First, restraints have been found to be independently associated with the development of delirium.(18,19) Second, restraints may exacerbate underlying hyperactive behavior. Finally, by restricting patients to bedrest, restraints further limit external stimuli, which in itself may increase the risk for delirium.(20)
Case & Commentary: Part 2
The doctor was called, and an arterial blood gas was performed. The patient's PaO2 was 91 mmHg, but the PaCo2 was 58 mmHg, a marked increase since admission. Despite the patient's deteriorating clinical condition, the patient's worsening level of consciousness was attributed to "senile dementia" and not impending respiratory failure (as evidenced by the significant carbon dioxide retention). No further action was taken. Over the course of the day, the patient developed worsening respiratory distress and became comatose, and eventually was transferred to the intensive care unit. She subsequently developed respiratory failure requiring intubation and renal failure requiring dialysis. Her condition did not significantly improve, and she eventually died 2 weeks later.
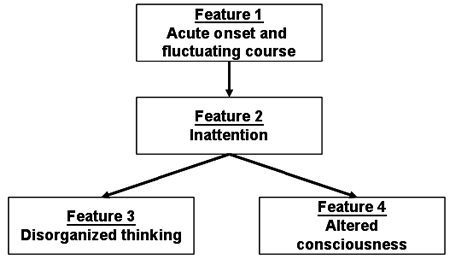
This patient was incorrectly diagnosed with dementia, despite a presentation most consistent with delirium. The diagnosis of delirium follows the diagnostic algorithm of the Confusion Assessment Method (CAM) and involves elements of history and physical examination.(21) The CAM algorithm has four features (Figure):
- Feature 1 is acute onset and fluctuating course. Presence of this feature can generally be obtained from family and nursing history.
- Feature 2, inattention, is assessed through brief cognitive assessment such as serial 7s (take the number 100 and subtract 7, keep going until I tell you to stop); digit span (I am going to read you some numbers and I want you to repeat them to me backwards); or asking the patient to recite months of the year or days of the week backwards.
- Feature 3, disorganized thinking, can be assessed via response to interview questions. For example, does the patient respond inappropriately or tangentially?
- Feature 4, disturbance of consciousness, helps identify the three psychomotor variants (hyperactive, hypoactive, mixed disorder).
Patients demonstrating features 1 and 2 along with either feature 3 or 4 should be considered to have delirium until proven otherwise.(11) The diagnosis of "senile dementia" is not appropriate in the setting of acute illness. The acute onset of confusion and hyperactivity in this case should have prompted cognitive assessment for inattention and disorganized thinking; such an assessment would likely have led to the correct diagnosis of delirium.
A thorough history and physical examination are required for patients suspected of having delirium. The neurological examination is especially important because while acute, focal neurological changes require neuroimaging, patients without such changes can usually have neuroimaging deferred, reserved for situations in which the cause cannot be determined from a medical/metabolic workup.(22) Core laboratory tests to identify electrolyte abnormalities, renal function, and infection (complete blood count and urinalysis) are warranted in all patients. The history and physical examination should guide further laboratory testing. An arterial blood gas was appropriately performed in this case, but it appears that the physician failed to tie the results (marked carbon dioxide retention) together with the patient's delirium.
All patients should have a thorough review of medications that may contribute to delirium, particularly benzodiazepines, anticholinergic medications, and psychoactive medications.(23) All medications that can precipitate delirium should be discontinued or have dosages lowered. Further consideration should be given to drugs that have recently been stopped and may cause a withdrawal syndrome (alcohol, chronic opioids, antidepressants, etc.).
Delirium is treated by identifying and remedying the underlying causes. Because of the associated morbidity and mortality, multiple causative pathways and treatments may need to be pursued and/or instituted simultaneously. Such causes might include electrolyte abnormalities, assessment of renal function, additional workup for other sources of infection (urinalysis or lumbar puncture if indicated), fecal impaction, and other myocardial/pulmonary causes of hypoxemia.
In this case, the best single explanation for the patient's deterioration is progressive pneumonia resulting in worsened gas exchange and carbon dioxide retention. Thus, delirium was likely the presenting symptom of impending hypercarbic respiratory failure. More aggressive treatment of the pneumonia and associated CO2 retention was warranted. Additionally, medication review should have been conducted, resulting in the removal of sedative or anticholinergic medications. It is unclear why further workup or treatment was not pursued in this case.
In this case, the patient's daughter was able to inform clinicians that her mother had never been confused or disoriented prior to hospitalization. In addition to their role in establishing the historical, behavioral, and cognitive baseline, family members and caregivers are an underutilized resource in the treatment of patients with delirium. For example, family members serve as a re-orienting stimulus for patients. In an average day on a hospital medical ward, 20-30 different staff members will enter a patient's room (nursing, nutrition, housekeeping, housestaff, consultants, attending physicians, etc.). As a result, patients with impaired cognition may misinterpret the in-room presence of these staff members, leading to paranoid thoughts and delusions. Family members or caregivers may be the only people whom the patient recognizes and, thus, can serve to reassure the patient about his or her current location and medical situation. Family or caregivers can also provide cognitive stimulation for the patient, such as by playing cards, doing crossword puzzles together, or viewing family photos. Additionally, family may be willing to participate in the care of the patient, which may reduce patient agitation, provide a constructive outlet for family concern, and decrease staff requirements.(24) As a result, family should be involved in the care of the delirious patient to the extent possible. Formal "visiting hours" may need to be relaxed or eliminated to ensure that the family is able to be present to calm the patient during periods of confusion.
The failure to recognize delirium in this patient may have delayed recognition of her worsening pneumonia, which in turn led to a failure to escalate the level of care. Cognitive assessment at admission and appropriate use of collateral information from the patient's daughter might have helped the physician realize that the patient's altered mental status represented delirium and not dementia. Delirium is associated with severe clinical consequences, so earlier recognition of delirium should have prompted a thorough search for precipitants and aggressive treatment of the underlying illness. Actively encouraging the family's participation in care may have helped identify delirium earlier and may have obviated the need for physical restraints in this case. In short, this patient's death may have been preventable with optimal care; as such, this case represents an instructive cautionary note.
Take-Home Points
- Delirium, an acute change in cognition and attention, is common, morbid, and costly.
- All change in mental status should be assumed to be delirium until proven otherwise.
- The treatment of delirium is to identify and remedy the underlying causes.
- Elements of the hospital environment can contribute to delirium and expose patients to safety risk.
- Family members and caregivers are crucial to the diagnosis and management of delirium. Incorporating their contribution into the plan of care is strongly recommended.
James L. Rudolph, MD, SM Assistant Professor of Medicine
Harvard Medical School
Associate Physician
Brigham and Women's Hospital
Staff Physician
VA Boston Healthcare System
Faculty Disclosure: Dr. Rudolph has declared that neither he, nor any immediate member of his family, has a financial arrangement or other relationship with the manufacturers of any commercial products discussed in this continuing medical education activity. In addition, the commentary does not include information regarding investigational or off-label use of pharmaceutical products or medical devices.
References
1. McNicoll L, Pisani MA, Zhang Y, Ely EW, Siegel MD, Inouye SK. Delirium in the intensive care unit: occurrence and clinical course in older patients. J Am Geriatr Soc. 2003;51:591-598. [go to PubMed]
2. Hustey FM, Meldon SW. The prevalence and documentation of impaired mental status in elderly emergency department patients. Ann Emerg Med. 2002;39:248-253. [go to PubMed]
3. Diagnostic and Statistical Manual of Mental Disorders, 4th ed, text revision. Washington, DC: American Psychiatric Association; 2000.
4. Inouye SK, Viscoli CM, Horwitz RI, Hurst LD, Tinetti ME. A predictive model for delirium in hospitalized elderly medical patients based on admission characteristics. Ann Intern Med. 1993;119:474-481. [go to PubMed]
5. Marcantonio ER, Goldman L, Mangione CM, et al. A clinical prediction rule for delirium after elective noncardiac surgery. JAMA. 1994;271:134-139. [go to PubMed]
6. Rudolph JL, Jones RN, Levkoff SE, et al. Derivation and validation of a preoperative prediction rule for delirium after cardiac surgery. Circulation. 2009;119:229-236. [go to PubMed]
7. Ely EW, Inouye SK, Bernard GR, et al. Delirium in mechanically ventilated patients: validity and reliability of the confusion assessment method for the intensive care unit (CAM-ICU). JAMA. 2001;286:2703-2710. [go to PubMed]
8. Chelluri L, Pinsky MR, Donahoe MP, Grenvik A. Long-term outcome of critically ill elderly patients requiring intensive care. JAMA. 1993;269:3119-3123. [go to PubMed]
9. Inouye SK, Schlesinger MJ, Lydon TJ. Delirium: a symptom of how hospital care is failing older persons and a window to improve quality of hospital care. Am J Med. 1999;106:565-573. [go to PubMed]
10. Inouye SK, Rushing JT, Foreman MD, Palmer RM, Pompei P. Does delirium contribute to poor hospital outcomes? A three-site epidemiologic study. J Gen Intern Med. 1998;13:234-242. [go to PubMed]
11. Inouye SK. Delirium in older persons. N Engl J Med. 2006;354:1157-1165. [go to PubMed]
12. Bergmann MA, Murphy KM, Kiely DK, Jones RN, Marcantonio ER. A model for management of delirious postacute care patients. J Am Geriatr Soc. 2005;53:1817-1825. [go to PubMed]
13. Franco K, Litaker D, Locala J, Bronson D. The cost of delirium in the surgical patient. Psychosomatics. 2001;42:68-73. [go to PubMed]
14. Leslie DL, Zhang Y, Bogardus ST, Holford TR, Leo-Summers LS, Inouye SK. Consequences of preventing delirium in hospitalized older adults on nursing home costs. J Am Geriatr Soc. 2005;53:405-409. [go to PubMed]
15. Leslie DL, Marcantonio ER, Zhang Y, Leo-Summers L, Inouye SK. One-year health care costs associated with delirium in the elderly population. Arch Intern Med. 2008;168:27-32. [go to PubMed]
16. Liptzin B, Levkoff SE. An empirical study of delirium subtypes. Br J Psychiatry. 1992;161:843-845. [go to PubMed]
17. Provision of care, treatment, and services. Standards 11.10-100. In: Comprehensive Accreditation Manual for Hospitals. The Joint Commission; 2008: PC-25-26. ISBN: 978-1599401263.
18. McCusker J, Cole M, Abrahamowicz M, Han L, Podoba JE, Ramman-Haddad L. Environmental risk factors for delirium in hospitalized older people. J Am Geriatr Soc 2001;49:1327-1334. [go to PubMed]
19. Inouye SK, Charpentier PA. Precipitating factors for delirium in hospitalized elderly persons. Predictive model and interrelationship with baseline vulnerability. JAMA. 1996;275:852-857. [go to PubMed]
20. Creditor MC. Hazards of hospitalization of the elderly. Ann Intern Med. 1993;118:219-223. [go to PubMed]
21. Inouye SK, van Dyck CH, Alessi CA, Balkin S, Siegal AP, Horwitz RI. Clarifying confusion: the confusion assessment method. A new method for detection of delirium. Ann Intern Med. 1990;113:941-948. [go to PubMed]
22. Hirano LA, Bogardus ST, Jr., Saluja S, Leo-Summers L, Inouye SK. Clinical yield of computed tomography brain scans in older general medical patients. J Am Geriatr Soc. 2006;54:587-592. [go to PubMed]
23. Fick DM, Cooper JW, Wade WE, Waller JL, Maclean JR, Beers MH. Updating the Beers criteria for potentially inappropriate medication use in older adults: results of a US consensus panel of experts. Arch Intern Med. 2003;163:2716-2724. [go to PubMed]
24. Cole MG, Primeau FJ, Bailey RF, et al. Systematic intervention for elderly inpatients with delirium: a randomized trial. CMAJ. 1994;151:965-970. [go to PubMed]
Table
Table. Delirium Prediction Rule for Patients Based on Admission Characteristics.(4)
| Feature (1 point each) | Measurement | Points |
|---|---|---|
| Cognitive impairment | MMSE | 1 |
| Acute illness | APACHE >16 | 1 |
| Visual impairment | Corrected >20/70 | 1 |
| Dehydration | Urea nitrogen:creatinine ≥18 | 1 |
The points are added. The incidence of delirium in patients scoring 0 points is 3-9%, 1-2 points is 16-23%, and for ≥3 points is 32-83%. MMSE, Mini Mental State Examination; APACHE, Acute Physiology, Age, and Chronic Health Evaluation.
Figure
Figure. The Confusion Assessment Method (CAM) for the diagnosis of delirium. Diagnosis of delirium using the CAM requires the presence of both features 1 and 2, and either feature 3 or 4.